At its core, methadone works by interacting with the same parts of the brain that other opioids do, but in a much more controlled and stable way. It’s what we call a long-acting opioid agonist. In simpler terms, it satisfies the brain's physical need for opioids, which effectively stops the agony of withdrawal and shuts down the intense cravings that drive the cycle of addiction.
This stability is the key. It’s what gives someone the breathing room to step off the rollercoaster of use and focus on their recovery.
Key Takeaways
- Methadone is a long-acting opioid agonist that provides stable, controlled effects.
- It works by satisfying the brain's physical need for opioids.
- The primary goals are to eliminate withdrawal symptoms and intense cravings.
- This stability allows individuals to focus on their recovery rather than just surviving.
- It is a medical treatment, not a substitute for illicit drug use.
How Methadone Calms the Brain and Body
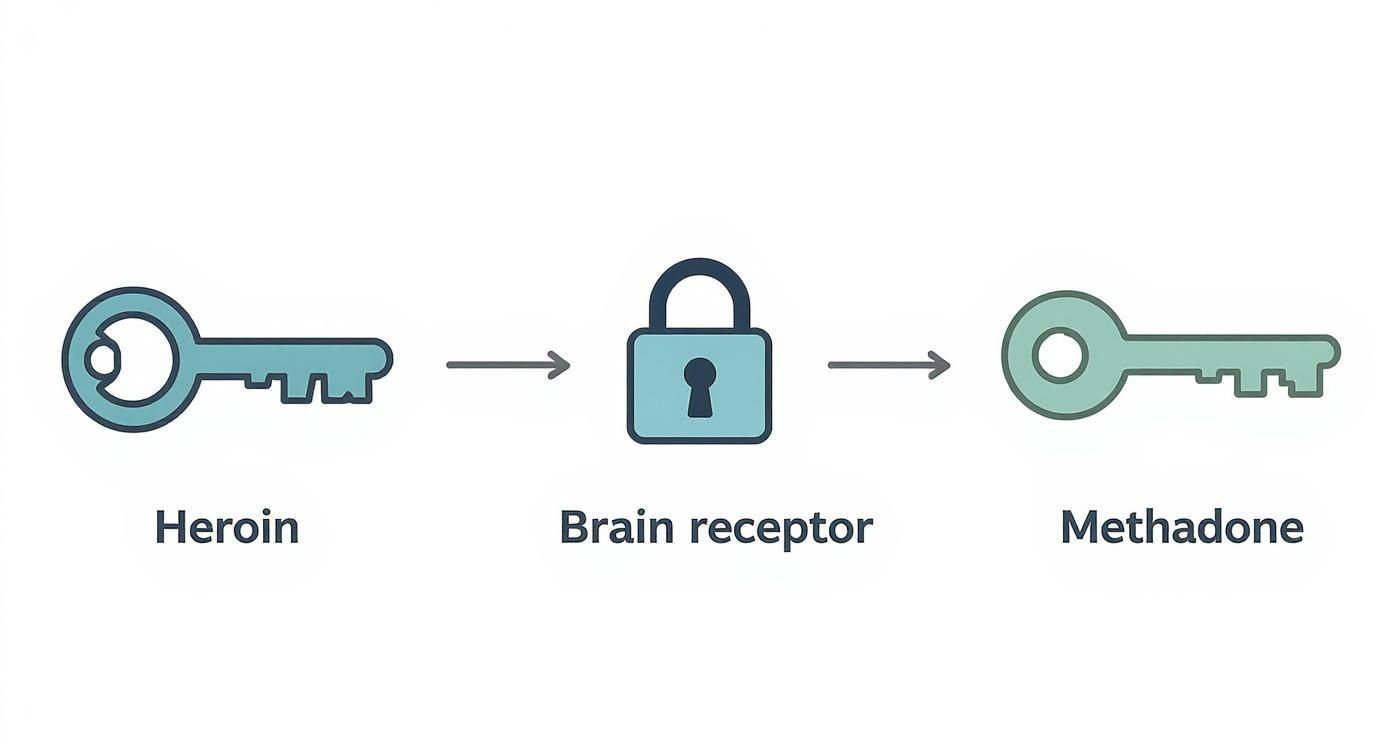
To really get how methadone works, you have to picture the opioid receptors in the brain. Think of them like tiny locks. Short-acting, powerful opioids like heroin or fentanyl are like master keys that violently burst the lock open. They deliver a powerful, short-lived high, but it's followed by an equally intense crash, which just fuels the desperate need to use again.
Methadone is a completely different kind of key. It's designed to fit the very same lock, but it turns it slowly and gently, keeping things stable for a long time—usually 24 to 36 hours from just one dose. This slow, steady action is precisely what makes it such a powerful medical tool.
The Science Behind a Stable Foundation
Instead of causing a euphoric rush, methadone provides a consistent, steady level of activation at the opioid receptors. This essentially tells the brain, "Everything is okay," which accomplishes two critical goals for someone in early recovery:
- It Stops Withdrawal Symptoms: By keeping the receptors occupied, methadone prevents the severe physical sickness (nausea, body aches, sweating) and psychological distress that come with opioid withdrawal.
- It Blocks Cravings: With the receptors satisfied, the overwhelming, compulsive urge to use opioids fades into the background, often disappearing completely.
This isn't just about making someone feel more comfortable. It’s about creating the biological foundation for real, lasting change. When a person is no longer trapped in the chaotic cycle of getting high just to avoid getting sick, they finally have the mental and emotional space to engage in counseling and start rebuilding their life.
Methadone provides the neurochemical stability needed for a person to break free from the compulsive, drug-seeking behaviors of addiction. It allows them to shift their focus from surviving the next few hours to planning a future.
Why It's a Tool for Recovery, Not a Substitute
It's a common misconception, but it’s crucial to understand that methadone used in a treatment program is medicine, not a replacement drug. While it is technically an opioid, its function is therapeutic. When taken as prescribed by a doctor, it doesn't cause a "high" or impairment.
Instead, it normalizes brain chemistry and body functions that have been thrown into disarray by opioid use disorder. This allows people to get back to their lives—to go to work, be present for their families, and reconnect with their communities.
Let's break down how it achieves this.
The table below summarizes the key ways methadone works in the brain to support recovery from opioid use disorder.
| Mechanism | How It Works in the Brain | The Benefit for Recovery |
|---|---|---|
| Opioid Agonist | Binds to and activates mu-opioid receptors, the same ones affected by heroin and fentanyl. | Satisfies the physical dependence, preventing the body from going into painful withdrawal. |
| Long-Acting | Has a long half-life, meaning it stays active in the body for 24-36 hours. | Allows for once-daily dosing and provides continuous relief from cravings and withdrawal symptoms. |
| Slow Onset | It's absorbed slowly, so it doesn't produce the rapid, euphoric "rush" of short-acting opioids. | Prevents the reinforcing high-crash cycle that drives addictive behavior. |
| Cross-Tolerance | At a stable dose, it can block the euphoric effects of other opioids if they are used. | Reduces the incentive for relapse, as taking other opioids will not produce the desired effect. |
This unique combination of properties is what makes methadone such an effective cornerstone of Medication for Opioid Use Disorder (MOUD).
Key Takeaways
- Methadone gently activates opioid receptors for 24-36 hours, preventing highs and lows.
- Its primary functions are to stop withdrawal symptoms and block drug cravings.
- It does not cause a "high" when taken at a stable, prescribed dose.
- It creates the biological stability needed for a person to engage in therapy.
- At a therapeutic dose, it can block the euphoric effects of other opioids.
Frequently Asked Questions
Is methadone just replacing one addiction with another?
Not at all. This is a common myth, but addiction is defined by compulsive, out-of-control drug use despite negative consequences. Medically prescribed methadone does the opposite: it restores control. It stabilizes brain chemistry without the high, allowing people to function normally and focus on therapy. It's medical treatment, not a substitute addiction.
How long does it take for methadone to start working?
After taking a dose, you'll typically start to feel its effects within 30 minutes. It reaches its peak effectiveness within a few hours, and its long-acting nature provides a full 24 hours or more of relief from both withdrawal and cravings.
Can you overdose on methadone?
Yes, a methadone overdose is possible, and it's very dangerous. The risk is highest when it's not taken as prescribed or when it's mixed with other central nervous system depressants, like alcohol or benzodiazepines (e.g., Xanax, Klonopin). This is precisely why methadone is dispensed in a highly controlled clinical setting, where medical staff can monitor dosing and ensure patient safety.
The Four Structured Phases of Methadone Treatment
Think of methadone treatment less as a single action and more as a structured medical journey. It's not a quick fix but a carefully managed process broken down into four distinct phases. Each stage has a clear purpose, designed to support you as you move toward lasting recovery, and the entire process is personalized to fit your specific physical and psychological needs.
This progression is all about moving from the crisis of acute physical dependence to building a solid foundation for long-term stability and a healthier life.
Phase 1: Induction
This is where it all begins. The induction phase is the carefully controlled start of your treatment. The main goal here is straightforward: find the lowest possible dose of methadone that stops the intense discomfort of opioid withdrawal. This initial period is often the most intensive part of the process, usually requiring daily visits to the clinic.
Under the watchful eye of a medical team, you’ll receive a small starting dose. The clinical staff will then monitor how you’re feeling over the next few hours, looking for signs that your withdrawal symptoms are easing. Over several days, the dose is gradually and safely increased until it reaches a therapeutic level—one that successfully holds off withdrawal and cravings without making you feel sedated or groggy.
The goal of induction isn’t to hit a specific number on a chart. It’s about finding the precise dose that brings your body back into balance. This careful, medically supervised process is crucial for your safety and sets the stage for everything that follows.
Phase 2: Stabilization
Once those initial withdrawal symptoms are under control, you move into the stabilization phase. The focus now shifts from simply stopping the sickness to fine-tuning your methadone dose. The new aim is to eliminate cravings completely and help you feel "normal" and functional all day long.
This phase might involve small, careful adjustments to your dosage. The medical team works closely with you to find that sweet spot—the optimal level that gives you 24-hour relief without any breakthrough cravings or lingering withdrawal symptoms. Hitting this point is a huge milestone. It frees you from the constant physical and mental pull of addiction, allowing you to finally start engaging fully with the counseling and therapy that are so essential to recovery.
This infographic helps visualize what's happening. Think of the brain's opioid receptors as a lock. A drug like heroin is a jagged key that forces the lock, causing chaos. Methadone is like a smooth, perfectly fitting key that turns the lock gently and keeps it securely occupied.
As the image shows, by safely occupying the receptor, methadone effectively blocks withdrawal and cravings, giving you the clear headspace you need to begin healing.
Phase 3: Maintenance
The maintenance phase is the long-term heart of methadone treatment. This is where the real, deep healing happens. With your dose stable, the medication works quietly in the background, providing the brain chemistry support you need to rebuild your life. For many people, this phase lasts for a year or much longer.
While in maintenance, you continue your daily dose, which makes it possible to:
- Focus on Therapy: You can dive deep into individual and group counseling to get at the root causes of addiction.
- Rebuild Relationships: This is your chance to work on repairing connections with family and friends.
- Pursue Life Goals: You can return to work, go back to school, find stable housing, and rediscover hobbies and interests.
The stability that methadone provides during this phase is what makes everything else possible. It allows you to develop healthy coping skills and build a fulfilling life, free from the shadow of opioids.
Phase 4: Tapering
After a significant period of stability, and only with the full support of your medical team, you might choose to begin the tapering phase. It’s critical to understand that this step is completely optional. Many people find that staying on methadone long-term is the best path for their recovery, and lifelong maintenance is a valid and often life-saving treatment.
If you and your doctor decide that tapering is the right move, your methadone dose will be reduced very, very slowly over months or even years. This gradual decrease allows your body to adjust without triggering a return of withdrawal symptoms or intense cravings. The decision to taper is a major medical one and should only be made after a lot of thought and in full partnership with your treatment team. The goal is always your long-term well-being, whether that includes continued methadone treatment or not.
Key Takeaways
- Induction: The starting phase where a safe, effective dose is found to stop withdrawal.
- Stabilization: The dose is fine-tuned to eliminate cravings and normalize body function.
- Maintenance: A long-term phase where the stable dose supports therapy and rebuilding one's life.
- Tapering: An optional phase where the dose is very slowly reduced under medical supervision.
- The entire process is medically supervised and personalized to individual needs.
Frequently Asked Questions
How long does treatment take?
The duration of methadone treatment is highly individual. Some people may stay on it for a year or two, while others benefit from long-term maintenance for many years. The decision is based on your stability and recovery goals, made in consultation with your medical team.
What happens if I miss a dose?
Missing one dose might cause you to feel some mild withdrawal symptoms, but because methadone is long-acting, the effects are usually not severe. It's important to contact your clinic immediately for guidance. Consistently missing doses will lead to a return of withdrawal and cravings.
The Proven Effectiveness of Methadone Treatment
It’s one thing to understand the science of how methadone works, but it’s another to see the real-world impact it has had for decades. This isn’t some experimental fix. Methadone is a gold-standard medical treatment, backed by an enormous body of evidence, that has proven to be one of the most powerful tools we have in the fight against the opioid crisis.
Major studies consistently show that people in methadone maintenance treatment have a dramatically lower risk of a fatal overdose. It also helps people stop using illicit opioids, breaking a destructive cycle and giving them the stability needed to rebuild their health and their lives.
A Powerful Public Health Tool
The ripple effect of methadone treatment goes far beyond the individual. It's a cornerstone of public health. By helping people stop or reduce the use of illicit opioids, especially those taken by injection, treatment programs also slash the transmission rates of infectious diseases like HIV and hepatitis C.
This community-wide benefit is a huge part of methadone's value. It helps protect entire communities while giving individuals a genuine chance to stabilize and begin the hard work of recovery.
The data is clear and compelling: patients engaged in methadone treatment have dramatically better outcomes than those who are not. It provides the stability necessary for a person to step away from the daily chaos of addiction and focus on long-term healing.
Backed by Decades of Research
The clinical evidence supporting methadone is rock-solid, built up over many years of research. Study after study has confirmed its success in keeping people in treatment and reducing heroin use. A landmark 2009 Cochrane review, which analyzed multiple randomized controlled trials, found methadone to be significantly more effective than treatment without medication.
The numbers are striking. One major review found that methadone treatment was associated with a 69 percent reduction in all-cause mortality among people with opioid use disorder. Another large-scale study saw that methadone was linked to a 76% reduction in overdose at three months and a 59% reduction at 12 months. You can explore the full research findings on methadone's life-saving impact.
This mountain of data simply confirms what clinicians have witnessed firsthand for decades. Methadone treatment isn’t a theory—it’s a life-saving medical practice that delivers tangible, measurable results for individuals, families, and communities.
Creating the Opportunity for Lasting Change
Ultimately, the power of methadone lies in its ability to build a foundation for recovery. It works by managing the overwhelming physical aspects of opioid dependence—the constant cravings and painful withdrawal.
By getting those under control, methadone frees up the mental and emotional space a person needs to truly engage with counseling, therapy, and other support. Trying to address the deep psychological roots of addiction while your body is in constant turmoil is an uphill battle, if not an impossible one. Methadone clears the way for that essential therapeutic work to begin, making long-term recovery an achievable goal.
Key Takeaways
- Reduces Overdose Risk: Extensive research shows that methadone maintenance dramatically lowers the risk of a fatal overdose.
- Decreases Illicit Opioid Use: It is incredibly effective at helping people stop using heroin and other illicit opioids.
- Improves Public Health: By curbing injection drug use, methadone helps limit the spread of diseases like HIV and hepatitis C.
- Enhances Treatment Retention: People on methadone are far more likely to stick with their recovery programs.
- Enables Comprehensive Recovery: Methadone provides the physical stability needed for a person to fully benefit from counseling and psychosocial support.
Frequently Asked Questions
Is methadone treatment effective?
Yes, extremely. Decades of research have proven that methadone treatment significantly reduces the risk of fatal overdose, decreases illicit opioid use, helps people stay in treatment longer, and reduces the transmission of diseases like HIV and hepatitis C. It is considered a gold-standard treatment for opioid use disorder.
How does methadone help the community?
Methadone treatment has broad public health benefits. By reducing illegal drug use and needle sharing, it lowers the rates of infectious diseases in the community. It also helps people become stable, return to work, and reconnect with their families, which benefits society as a whole.
Comparing Methadone, Buprenorphine, and Naltrexone
While methadone is a powerful tool for treating opioid use disorder, it's not the only one in the toolbox. Understanding how it stacks up against the other main options—buprenorphine and naltrexone—is key to making an informed choice about your recovery journey.
Each medication works differently, which impacts everything from where you get it to who it's best suited for. Let's break down the differences so you can have a more productive conversation with your doctor about what’s right for you.
How Each Medication Works in the Brain
The easiest way to grasp the difference is by thinking of your brain's opioid receptors as locks. Each medication acts like a different kind of key.
-
Methadone (Full Agonist): Think of this as a master key that fits the lock perfectly and turns it all the way. It fully activates the opioid receptors, but it does so slowly and in a controlled way. This action satisfies the body's physical dependence, effectively stopping withdrawal and cravings without producing the euphoric "high" when taken as prescribed.
-
Buprenorphine (Partial Agonist): This key fits the lock but only turns it partway. It gives the receptors just enough stimulation to ward off withdrawal and cravings, but it has a built-in "ceiling." That means after a certain dose, its opioid effects don't increase, which significantly lowers the risk of misuse and overdose.
-
Naltrexone (Antagonist): This is more like a shield that blocks the keyhole entirely. It binds to the opioid receptors but doesn't activate them at all. Instead, it prevents any other opioids from attaching, meaning someone taking naltrexone won't be able to feel the effects of heroin or fentanyl if they use them.
This core difference is why a full agonist like methadone is often the go-to for people with a high level of physical dependence.
Different Medications, Different Treatment Paths
Because these medications work so differently, the treatment experience for each one is unique. The right choice really hinges on a person's history with opioids, their daily life, and what they hope to achieve in recovery.
For example, methadone can only be dispensed at federally regulated Opioid Treatment Programs (OTPs), which usually means daily visits, especially when you're just starting. Buprenorphine, on the other hand, can be prescribed by a certified doctor and picked up at a pharmacy, offering a lot more flexibility.
Naltrexone has a critical requirement: you must be completely free of all opioids for 7 to 14 days before the first dose. Taking it too soon can trigger immediate, intense withdrawal. This makes it a better fit for people who have already detoxed and are focused on preventing relapse.
These practical details matter. If daily clinic visits are a major roadblock, buprenorphine might be a better fit. But for someone who thrives with the structure and accountability of a clinic setting, methadone provides a solid foundation for recovery. You can get a deeper look at what is Medication-Assisted Treatment to see how these options fit into a comprehensive plan.
A Side-by-Side Look
The best way to see the contrasts is to put them head-to-head. The table below breaks down the key features of each medication, helping to clarify their distinct roles in treating opioid use disorder.
Comparison of Medications for Opioid Use Disorder
| Feature | Methadone | Buprenorphine (Suboxone) | Naltrexone (Vivitrol) |
|---|---|---|---|
| Mechanism | Full Opioid Agonist | Partial Opioid Agonist | Opioid Antagonist |
| Primary Goal | Stop withdrawal, eliminate cravings | Reduce withdrawal, reduce cravings | Block opioid effects, prevent relapse |
| Dispensing | Specialized OTP clinics (daily visits) | Certified doctors' offices (prescriptions) | Any licensed healthcare provider |
| Overdose Risk | High if misused | Lower (due to ceiling effect) | Very low (non-opioid) |
| Prerequisites | Can be started during withdrawal | Must be in mild withdrawal to start | Must be opioid-free for 7-14 days |
Ultimately, there is no single "best" medication. The most effective choice is the one that aligns with your specific medical needs, lifestyle, and recovery goals. The only way to know for sure is to have a thorough assessment with a healthcare professional.
Key Takeaways
- Methadone is a full agonist, buprenorphine is a partial agonist, and naltrexone is an antagonist.
- Methadone is ideal for managing severe withdrawal and cravings.
- Buprenorphine offers more flexibility as it can be prescribed by a doctor.
- Naltrexone is for relapse prevention and requires a person to be fully detoxed first.
- The best medication choice is personal and depends on individual needs and circumstances.
Frequently Asked Questions
Is one medication better than the others?
Not at all. The right medication is deeply personal. It depends on factors like your history of opioid use, your physical health, your daily responsibilities, and your support system. What works wonders for one person might be the wrong choice for another.
Can I switch from one medication to another?
Yes, but this has to be done carefully and under the guidance of a doctor. Moving between medications—say, from methadone to buprenorphine—is a structured process designed to manage withdrawal and keep you safe.
Do these medications cure opioid addiction?
No, they are treatments, not cures. Think of them as tools that stabilize your brain and body, giving you the clarity and freedom from cravings needed to do the real work of recovery in counseling and therapy. They address the physical side so you can focus on the psychological and behavioral aspects of addiction.
The Vital Role of Counseling in Recovery
Methadone is a game-changer for stabilizing the body, but real, lasting recovery goes much deeper than just managing physical symptoms. A good way to think about it is that methadone builds a solid foundation, which is absolutely essential. But it's counseling that builds the actual house. To truly heal, you have to address the psychological and behavioral patterns that drove the addiction in the first place, and that’s where therapy becomes indispensable.
While the medication gets to work stopping cravings and preventing withdrawal, counseling gives you the tools to start rebuilding your life. It creates a safe, confidential space to dig into the root causes of substance use, process underlying trauma, and begin repairing relationships that addiction may have damaged. This combination of medication and therapy is the gold standard because it treats the whole person—mind and body together.
Building Skills for a Life Beyond Addiction
A comprehensive methadone program doesn't just dispense medication; it integrates psychosocial support to arm you with practical skills for navigating life without opioids. Therapy sessions are designed to help you pinpoint your triggers, develop healthier ways to cope, and start changing the thought patterns that lead to self-destructive choices.
This is the work that teaches you how to handle stress, manage tough emotions, and communicate more effectively with the people in your life. It’s not just about stopping drug use. It's about building a meaningful life where you no longer feel the need for them.
Methadone treatment opens a critical window of opportunity. By providing physical stability, it clears the way for the deep, therapeutic work that is necessary for long-term recovery to take hold.
Cognitive Behavioral Therapy and Group Support
One of the most effective and widely used therapeutic methods is Cognitive Behavioral Therapy (CBT). It’s built on the idea that our thoughts, feelings, and actions are all connected. By learning to challenge and reframe negative thinking, you can fundamentally change how you respond to stressful situations that used to be triggers. To learn more, you can explore our guide on the powerful role of CBT in addiction treatment and see how it fosters lasting change.
Beyond one-on-one sessions, group counseling offers its own powerful benefits:
- Shared Experience: There's immense power in connecting with others who just get it. It melts away the feelings of isolation and shame that addiction thrives on.
- Accountability: Being part of a group creates a supportive network that helps keep you accountable to yourself and your recovery goals.
- New Perspectives: Hearing how other people navigated similar challenges can give you incredible insights and fresh ideas for your own journey.
This powerful blend of medication and robust psychosocial support is what elevates methadone treatment from a temporary solution to a true pathway for sustainable recovery.
Key Takeaways
- Methadone Creates Stability: The medication handles the physical side of addiction by stopping cravings and withdrawal, letting you focus on healing.
- Counseling is Essential: Therapy is where you do the work to address the psychological and behavioral roots of substance use disorder.
- It Builds Coping Skills: You learn real-world tools to manage stress, triggers, and difficult emotions without falling back on old habits.
- Therapy Heals the Whole Person: Combining medication with counseling provides a complete, holistic approach to recovery.
- Group Support is Powerful: Sharing your experience with peers breaks down isolation and builds a strong community for long-term success.
Frequently Asked questions
Is counseling mandatory in a methadone program?
Yes, federal regulations require that all patients in an Opioid Treatment Program (OTP) receive counseling and other support services. Decades of evidence have shown that this combined approach is, by far, the most effective model for treating opioid use disorder.
What kind of therapy will I get?
Most programs offer a mix of individual counseling, group therapy, and often family therapy. The specific approach, like using Cognitive Behavioral Therapy (CBT) or Dialectical Behavior Therapy (DBT), will be matched to your unique needs and outlined in your personal treatment plan.
How often do I have to attend counseling?
The frequency really depends on where you are in your recovery journey and the program's structure. When you're just starting out, you can expect sessions to be more frequent. As you become more stable and confident, the schedule often becomes more flexible, but that ongoing support remains a crucial part of the treatment.
The Bottom Line on Methadone Treatment
When you boil it all down, understanding how methadone treatment works is the first step toward seeing its incredible, life-saving potential. For so many people, this medication has been the bedrock of their recovery, giving them the stability they needed to put the pieces of their life back together, free from opioid use disorder.
If you remember nothing else, keep these key points in mind:
-
It Calms the Brain. Methadone is what's called a long-acting opioid agonist. In simple terms, it settles into the same brain receptors that other opioids would, effectively stopping withdrawal and shutting down cravings—all without producing the "high."
-
It Opens the Door to Real Recovery. Once the intense physical symptoms are managed, you finally have the space to breathe and focus. This is when the real work can begin, allowing you to fully engage in the counseling and therapy that are crucial for long-term healing.
-
The Proof Is in the Numbers. Decades of research have shown, without a doubt, that methadone treatment dramatically reduces the risk of a fatal overdose. It’s also incredibly effective at helping people stop using illicit opioids.
-
It’s a Carefully Guided Medical Journey. This isn't a one-and-done prescription. Treatment is a structured process with distinct phases—from starting on the medication (induction) to finding the right dose (stabilization) and staying on it for as long as needed (maintenance). For some, it might eventually include a slow, medically supervised taper.
-
It's One of Several Strong Options. Methadone is a powerful tool in the fight against opioid use disorder, but it's not the only one. It sits alongside other proven medications like buprenorphine and naltrexone, giving people different paths to find what works best for them.
Key Takeaways
- Methadone works by stabilizing the brain, stopping withdrawal, and ending cravings.
- It provides the physical foundation necessary for counseling and therapy to be effective.
- Treatment is a structured, phased medical process supervised by professionals.
- It is a scientifically proven method to reduce overdose deaths and illicit drug use.
- Methadone is one of several effective medication options for opioid use disorder.
Frequently Asked Questions About Methadone Treatment
Here are answers to some of the most common questions people have when considering methadone treatment.
How Long Will I Be on Methadone?
There’s really no one-size-fits-all answer here. For some people, methadone is a tool they use for a year or two to get back on their feet and build a solid foundation in recovery. For others, staying on methadone long-term is what works best to maintain stability and prevent relapse. The decision to eventually taper off is a major medical choice. It's a slow, careful process that you and your doctor decide on together, only when you both feel confident that you’re stable and truly ready.
Will Methadone Make Me Feel "High"?
This is a huge misconception. When you're on a stable, therapeutic dose prescribed by a clinic, methadone does not produce a euphoric high. Instead, it works in the background to normalize your brain chemistry. The goal is to eliminate withdrawal symptoms and quiet the constant drug cravings. This frees you up to think clearly, go to work, take care of your family, and just live your life without the constant fight against opioid use disorder.
Can I Just Get a Prescription From My Family Doctor?
Unlike other medications, you can't get a methadone prescription for addiction treatment from your regular doctor's office. It can only be provided through specially regulated clinics, which you'll hear called Opioid Treatment Programs (OTPs) or simply "methadone clinics." This highly structured system is designed for safety. It involves daily visits at first and makes sure that counseling and other support services are built right into your treatment plan. This integrated approach is a core part of what makes methadone treatment work safely and effectively.
Unfortunately, getting to one of these clinics can be a real challenge. In the United States, only 25.1% of adults who needed treatment for opioid use disorder in 2022 were able to get medication-assisted options. In stark contrast, countries like Switzerland have seen much lower overdose rates by making methadone far more accessible. You can learn more about these treatment gaps from the CDC's analysis.
Is Methadone Safe During Pregnancy?
Yes. In fact, methadone is the recommended standard of care for pregnant individuals with opioid use disorder. It is much safer for both the parent and the baby than continued illicit opioid use or trying to detox without medical support, which can cause severe complications. Treatment under a doctor's care helps stabilize the pregnancy and increases the chances of a healthy outcome.
What Are the Common Side Effects?
Like any medication, methadone can have side effects. In the beginning, some people may experience drowsiness, lightheadedness, or constipation. Most of these side effects are mild and tend to decrease as your body adjusts to a stable dose. It's important to communicate openly with your medical team about any side effects you're experiencing.