A Dallas resident may already know the pattern. Work piles up. Tasks start but don’t finish. Sleep slips. Alcohol, cannabis, stimulants, or pills start to feel like a shortcut to calm down, wake up, or get through the day. Then a harder question shows up. Is this untreated ADHD, addiction, or both?
That question matters because ADHD is a medical condition, not a character flaw. It can also overlap with substance use in ways that make self-diagnosis risky. Some people are trying to focus and accidentally worsen anxiety. Others are in recovery and scared that ADHD treatment will just replace one problem with another. Families across Dallas, Plano, Irving, Arlington, and the broader DFW area often arrive at the same crossroads.
This guide is built for that moment. It explains stimulant and non stimulant adhd medication in plain language, with close attention to the practical decisions that come up when addiction risk is part of the picture.
Table of Contents
- Understanding ADHD and the Path to Treatment in Dallas
- Explaining Stimulant Medications for ADHD
- Exploring Non-Stimulant ADHD Medication Options
- Stimulants vs Non-Stimulants A Detailed Comparison
- ADHD Medication and Substance Use Disorder A Critical Guide
- When to Seek Dual Diagnosis Treatment in Dallas
- FAQs About ADHD Medication and Recovery
Understanding ADHD and the Path to Treatment in Dallas
In Dallas, untreated ADHD often hides behind other labels. A person may look disorganized, unreliable, restless, impulsive, or emotionally reactive. In reality, that same person may be working twice as hard as everyone around them just to stay on track.
What ADHD often looks like in adult life
ADHD doesn’t always look like obvious hyperactivity. In adults, it may show up as missed deadlines, poor follow-through, chronic procrastination, overspending, traffic tickets, job instability, emotional frustration, or using substances to regulate energy and mood.
For readers who want a basic overview of common adult symptoms and how they can affect daily function, this primer on understanding ADHD in adults offers a useful starting point.
Many people in North Dallas, Oak Lawn, Lakewood, and nearby communities don’t seek help until consequences pile up. Sometimes the trigger is a relationship crisis. Sometimes it’s a relapse. Sometimes it’s realizing that sobriety is harder to maintain because the focus problems never went away.
Why treatment decisions feel complicated
ADHD treatment sounds simple from a distance. In practice, it isn’t. Medication can help, but the right choice depends on more than the diagnosis alone.
A safe plan has to account for:
- Symptom pattern: Some people struggle most with inattention. Others deal more with impulsivity, agitation, or emotional swings.
- Addiction history: A history of misusing alcohol, stimulants, opioids, or sedatives changes the risk discussion.
- Daily schedule: Work hours, parenting demands, sleep problems, and therapy participation all matter.
- Other conditions: Anxiety, depression, trauma, and bipolar symptoms can complicate medication response.
ADHD treatment should make life steadier. If a medication plan creates more chaos, cravings, secrecy, or instability, it needs to be reassessed.
For people seeking addiction treatment in Dallas, the goal isn’t just better concentration. It’s a treatment plan that supports both attention and recovery without adding unnecessary risk.
Explaining Stimulant Medications for ADHD
Stimulants are the most familiar ADHD medications. They work by increasing activity in brain systems involved in attention, task initiation, and self-regulation. A simple way to think about them is this. They turn up the volume on the brain’s focus signals so important tasks are easier to notice and stick with.
The main stimulant families
Most stimulant prescriptions fall into two groups.
- Methylphenidate-based medications: These are commonly used in ADHD treatment and include short-acting and extended-release versions.
- Amphetamine-based medications: These also come in short-acting and long-acting forms and are widely prescribed in adults.
Prescription patterns have stayed heavily weighted toward stimulants. From 2011 to 2013, stimulant prescribing declined from a peak of 68% and then remained stable at 61 to 64% through 2021, with methylphenidate most common in children and amphetamine products more common in adults, according to this prescribing trends review.
That pattern reflects a basic clinical reality. Stimulants often work quickly and can produce noticeable symptom relief when the medication and dose fit the person.
Short-acting versus long-acting forms
The same medication class can behave very differently depending on formulation.
Short-acting stimulants come on faster and wear off sooner. Some people like the flexibility. Others feel a sharper rise and drop.
Long-acting stimulants are designed to last through more of the day. They may reduce the need for repeat dosing and can feel smoother for some patients.
That difference matters in real life. A parent trying to manage work, school pickup, and evening responsibilities may need steadier coverage than someone who only needs support during a few focused hours.
What tends to work well
Stimulants can be especially useful when the main problem is severe distractibility, poor task persistence, mental fog, or frequent impulsive mistakes. People often report that routine tasks feel more doable. They’re not “smarter” on medication. They’re better able to direct attention where it needs to go.
Common clinical advantages include:
- Fast feedback: Response can often be assessed quickly.
- Flexible formulation options: Shorter and longer coverage windows are available.
- Stronger symptom effect for some patients: Especially when ADHD symptoms are pronounced.
What often doesn’t work well
Stimulants aren’t a match for everyone. Trouble usually starts when the medication causes insomnia, appetite suppression, jitteriness, emotional flattening, or a cycle of chasing performance rather than building stability.
Problems also show up when a person uses a prescribed stimulant in a way it wasn’t intended to be used. Taking extra doses, saving pills for stressful days, combining them with alcohol, or using them to compensate for sleep deprivation are warning signs.
A stimulant is treatment when it improves structure and functioning. It becomes a problem when the person starts organizing life around the medication itself.
For someone with a history of addiction, the medication class isn’t the only issue. Monitoring, timing, dose discipline, and the broader recovery plan matter just as much.
Exploring Non-Stimulant ADHD Medication Options
Non-stimulant ADHD medications offer a different path. They don’t create the same fast shift in attention that many people notice with stimulants. Instead, they tend to work more gradually and often require consistent daily use before benefits become clear.
That slower build can frustrate patients who want quick relief. It can also make non-stimulants a strong option for people who need steadier coverage or want to avoid the misuse concerns tied to controlled substances.
How non-stimulants work
This category includes medications that affect norepinephrine pathways or calm certain signaling systems involved in impulsivity and hyperarousal. The effect is usually less dramatic at the start.
Common non-stimulant options include medications such as atomoxetine, guanfacine, clonidine, and other newer non-stimulant formulations used in ADHD care. Each has a slightly different role.
Some are chosen when the main issue is classic inattentive ADHD. Others may be considered when ADHD overlaps with sleep problems, emotional reactivity, or a history that makes stimulant prescribing more complicated.
Why they matter more than many people assume
Non-stimulants are sometimes treated like backup options. That’s too simplistic. For some patients, they fit better from the start.
They may be considered when:
- Misuse risk is a serious concern: This matters in dual-diagnosis settings.
- Sleep or appetite is already fragile: Side effect priorities can shift the decision.
- Anxiety symptoms are prominent: A gentler medication profile may be easier to tolerate.
- The patient needs all-day consistency: Some non-stimulants provide a more even effect.
A separate public health issue is access. A meta-analysis found that only 19% of diagnosed children and adolescents receive pharmacological treatment overall, with rates above 40% in the US and below 10% in some other countries, as summarized in this review of global ADHD undertreatment. That gap matters because many families still don’t realize there are multiple medication pathways, not just one.
What patients need to know before starting
The biggest mistake with non-stimulants is quitting too early. Because they don’t usually produce an immediate shift, patients may assume they aren’t working when the medication hasn’t had enough time.
A safer expectation looks like this:
- Take it consistently. Skipping doses makes it hard to judge benefit.
- Track sleep, mood, attention, and irritability. Small gains can be easy to miss day to day.
- Review side effects early. Sedation or low energy may need adjustment.
- Give the plan time. These medications reward patience more than stimulants do.
For readers who are weighing how ADHD medication choices interact with anxiety symptoms, this related guide on https://dallasdetox.com/blog/adhd-medication-for-anxiety/ can help frame that conversation.
Non-stimulants aren’t weaker in every case. They’re different. For some people, that difference is exactly what makes them safer and more sustainable.
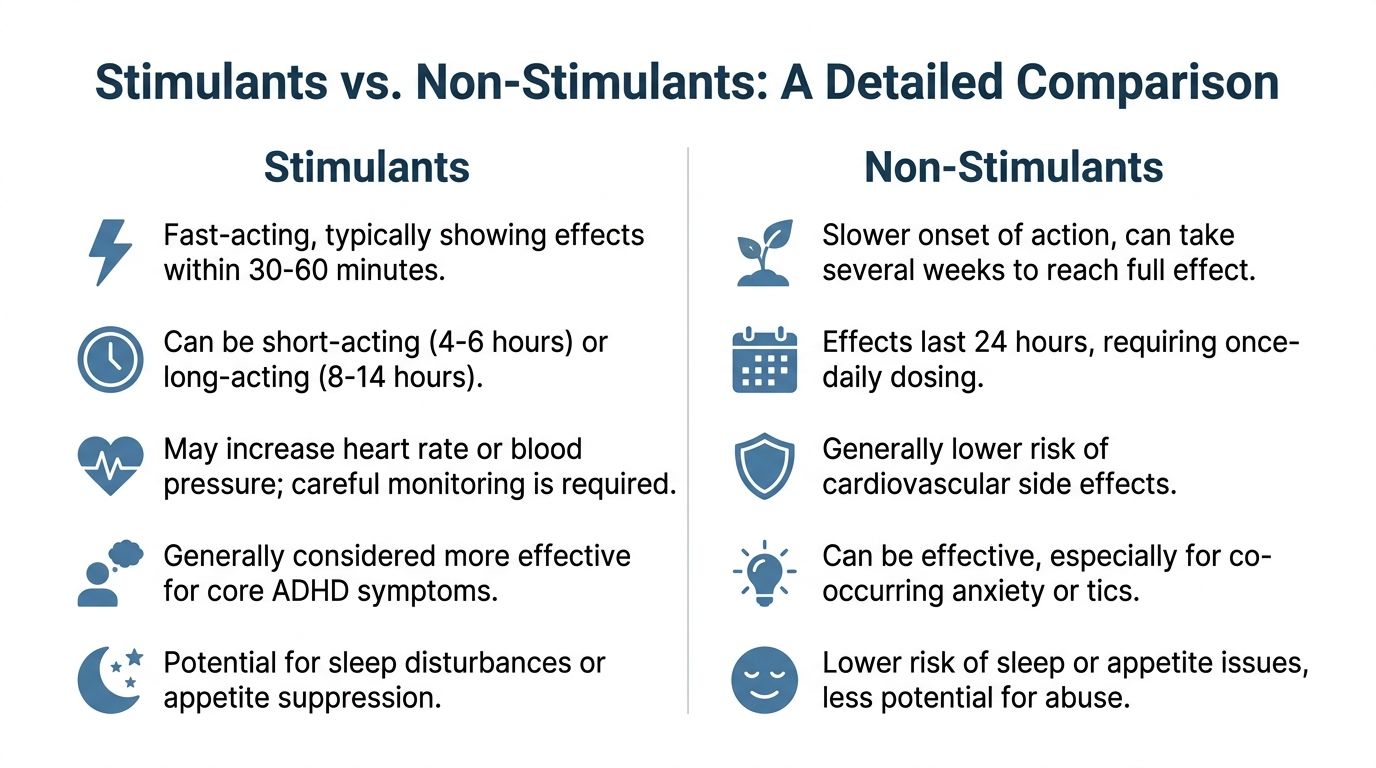
Stimulants vs Non-Stimulants A Detailed Comparison
A Dallas patient in early recovery may sit in my office and ask a very fair question. Will ADHD treatment help me function, or am I about to trade one problem for another? That question should shape the medication discussion from the start.
Both medication types can help. The safer choice depends on symptom pattern, side effects, daily demands, and relapse risk.
Key differences at a glance
| Factor | Stimulants | Non-stimulants |
|---|---|---|
| Typical onset | Often faster | Usually slower and more gradual |
| Daily feel | Can feel more noticeable | Often feels steadier once established |
| Misuse concern | Higher concern in vulnerable patients | Lower abuse potential |
| Common trade-off | Appetite and sleep issues may show up | Sedation or daytime sleepiness may show up |
| Best fit for some patients | Need rapid symptom relief | Need lower misuse risk or smoother coverage |
Efficacy and onset speed
Stimulants usually work faster than non-stimulants. Short-acting stimulant medications can start helping within about 30 minutes, while non-stimulants often need several weeks of regular use before the full benefit is clear, as explained in this review of stimulant and non-stimulant response differences.
That difference matters in real life. A person who is missing work deadlines, driving impulsively, or struggling to manage basic tasks may need symptom relief sooner.
Speed still does not settle the whole decision. In practice, side effects often determine the final medication choice. Some patients do very well on a fast-acting medication. Others stay on treatment longer with a slower option that feels steadier and creates less tension around sleep, appetite, or cravings.
Side effect patterns
The trade-offs are usually predictable. Stimulants more often create appetite loss, jitteriness, or insomnia. Non-stimulants more often cause fatigue, sleepiness, or a flat feeling early on.
Those patterns matter more in dual-diagnosis care than many patients expect.
A patient who already skips meals, struggles with anxiety, or has a history of using alcohol or cannabis to force sleep may have a harder time with a stimulating medication. A patient who is already low-energy, depressed, or foggy may stop a sedating medication before it has a chance to help. I often tell patients that the best medication on paper is not the best medication if it disrupts eating, sleep, or daily stability.
Common decision points include:
- Work and driving needs: Sedation can interfere with morning functioning and safety.
- Sleep vulnerability: Activating medications can worsen insomnia in some patients.
- Nutrition and weight: Appetite suppression can affect mood, energy, and recovery.
- Adherence: A medication that feels unpleasant is less likely to be taken correctly.
Misuse risk and recovery concerns
This is the part that deserves honest discussion, especially for people seeking treatment in Dallas for both ADHD and substance use disorder.
Stimulants can be appropriate in some dual-diagnosis cases, but they require more structure. Active cravings, a history of taking more than prescribed, or a pattern of using substances to control focus, energy, or mood all raise the risk. In those cases, non-stimulants often offer a safer starting point because they have lower abuse potential and less immediate reinforcement.
That does not mean stimulant treatment is automatically wrong for a person in recovery. It means the plan has to fit the level of risk. Long-acting formulations, close follow-up, family involvement when appropriate, pill counts, and regular review of cravings can all matter.
Alcohol is a common blind spot here. Patients sometimes underestimate how dangerous it is to mix a prescribed stimulant with drinking. If that risk is part of your history, this guide on mixing alcohol and Adderall is worth reading before any medication decision.
Family impact matters too. ADHD symptoms, relapse, poor supervision, and prescription misuse can spill into parenting and home safety. For families under stress, the connection between substance abuse and child neglect is part of the larger picture.
Coverage through the day
Symptom timing also changes the recommendation.
Some patients mainly need help during work or school hours. Others need coverage into the evening because ADHD affects parenting, arguments at home, driving, financial decisions, and the ability to follow through after the workday ends. Stimulants can offer flexible timing through short-acting or long-acting versions, but some patients notice clear peaks and drop-offs. Non-stimulants often feel more even across the day, which can be useful for patients who want steadier symptom control and less of a noticeable shift.
The practical comparison is simple.
- Stimulants: faster effect, more noticeable benefit for many patients, more caution needed if misuse risk is present
- Non-stimulants: slower build, steadier feel for some patients, often easier to consider when recovery stability is the priority
The right choice is the one a patient can use safely, consistently, and without undermining recovery.
ADHD Medication and Substance Use Disorder A Critical Guide
ADHD and substance use disorder can intensify each other. Untreated ADHD may drive impulsive decisions, poor frustration tolerance, and constant attempts to self-medicate. At the same time, substance use can mimic or worsen attention problems, making diagnosis messy.
That’s why medication decisions need more caution when addiction is in the picture.
Why dual diagnosis changes the decision
A patient with no history of substance misuse and a patient in early recovery don’t face the same prescribing question.
In dual-diagnosis care, the team has to ask:
- Is the patient stable enough to manage a controlled medication safely
- Are cravings active
- Has the person ever taken more than prescribed
- Does the patient use substances to manage sleep, energy, or mood
- Would a slower, lower-risk option support recovery better
Higher doses aren’t automatically better. Network meta-analyses found that unlicensed or higher stimulant doses may produce only marginal symptom reduction while carrying a doubled risk of dropout due to adverse events, with OR 2.02, according to this JAMA Psychiatry analysis. In real terms, chasing more effect can cost stability.
That matters in recovery. A medication plan should reduce chaos, not increase it.
What safe prescribing looks like
Safe treatment usually means structure. It rarely means handing over a prescription and hoping for the best.
A stronger approach often includes:
- Clear diagnosis before medication changes: Substance effects and withdrawal can look like ADHD.
- One prescriber or one coordinated team: Mixed messages create risk.
- Frequent follow-up: Early review catches misuse, side effects, or worsening mental health.
- Functional goals: The target isn’t feeling “more productive” in a vague way. It’s better sleep, safer routines, improved work performance, and lower relapse risk.
For families worried about the specific dangers of combining stimulants and alcohol, this page on https://dallasdetox.com/blog/mixing-alcohol-and-adderall/ addresses a common and risky pattern.
Family stress is often part of the picture
Substance use rarely affects one person alone. Parents, spouses, and children often absorb the instability long before treatment begins.
When family members are trying to understand how addiction can spill into neglect, home disruption, and legal risk, this article on the connection between substance abuse and child neglect can help clarify the broader consequences.
A person doesn’t need to wait for that level of damage before getting help. If ADHD symptoms and substance use are feeding each other, specialist care is warranted early.
When to Seek Dual Diagnosis Treatment in Dallas
Some people can manage ADHD treatment through routine outpatient care. Others need a setting that can address both substance use and mental health at the same time. The difference usually becomes clear when medication questions are tangled up with relapse, dishonesty, unsafe combinations, or worsening function.
Signs the situation needs specialist care
A Dallas-area patient may need dual diagnosis treatment if any of these sound familiar:
- Sobriety keeps slipping: Each attempt to quit alcohol or drugs falls apart because restlessness, impulsivity, or overwhelm becomes unbearable.
- Prescription use no longer feels controlled: The person takes extra doses, runs out early, hides pills, or mixes medication with other substances.
- Mood and attention are both unstable: It’s no longer clear what belongs to ADHD, anxiety, depression, trauma, withdrawal, or medication effects.
- Home life is becoming unmanageable: Arguments, missed responsibilities, job problems, and secrecy are escalating together.
- Primary care isn’t enough: The case needs closer psychiatric and addiction oversight than a brief medication visit can provide.
These situations are common across Dallas-Fort Worth, including communities such as Euless, Grapevine, Irving, Grand Prairie, and Arlington. Geography isn’t the issue. Complexity is.
The right level of care is the one that can treat both problems at once. Treating addiction while ignoring ADHD often fails. Treating ADHD while ignoring addiction can be dangerous.
What integrated treatment should include
A strong dual-diagnosis plan should do more than detox the body. It should create a safe framework for the decisions that come next.
Key elements include:
- Medical stabilization when alcohol, benzodiazepines, opioids, or other drugs are involved.
- Careful psychiatric evaluation after acute intoxication or withdrawal clears enough to assess symptoms accurately.
- Medication planning that considers misuse risk, side effects, sleep, cravings, and co-occurring disorders.
- Therapy for coping and structure so medication isn’t the only tool carrying the load.
- Relapse prevention built around real triggers such as boredom, shame, pressure, disorganization, and emotional overload.
For readers looking at treatment options that specifically address both psychiatric symptoms and substance use, this overview of https://dallasdetox.com/what-we-treat/dual-diagnosis-rehab/ explains what integrated care is meant to do.
When stimulant and non stimulant adhd medication decisions are being made in the middle of addiction recovery, specialist coordination isn’t a luxury. It’s the safer route.
FAQs About ADHD Medication and Recovery
A common question in Dallas treatment is simple and loaded at the same time. “If I have ADHD and a history of addiction, am I setting myself up for relapse if I take medication?” The honest answer is that some people can use ADHD medication safely in recovery, and some should not. The decision depends on diagnostic clarity, current sobriety, past stimulant misuse, active cravings, and how closely the prescribing team can monitor use.
Can someone in recovery ever take stimulant medication safely
Yes, in some cases. I only consider that option when the ADHD diagnosis is clear and the recovery plan is stable enough to support careful follow-up. A stimulant can help the right patient function better at work, think more clearly, and stop chasing relief through alcohol or other drugs. It can also become a problem if the person is using it to stay awake, push through emotional crashes, or recreate a high.
That trade-off matters. In dual-diagnosis care, the goal is not just symptom relief. The goal is symptom relief without feeding relapse.
Are non-stimulants addictive
Non-stimulants are usually preferred when misuse risk is a concern because they carry far less abuse potential. That makes them a safer starting point for many people with both ADHD and substance use disorder.
They still require real medical oversight. Non-stimulants can cause side effects, may take longer to work, and do not help every patient equally. Lower addiction risk does not mean automatic fit.
Will treating ADHD make sobriety easier or harder
Either outcome is possible. Well-managed ADHD treatment can reduce overwhelm, impulsive behavior, and the urge to self-medicate. Poorly managed treatment can worsen insomnia, anxiety, appetite changes, or medication boundary problems, which puts recovery under strain.
I often tell families to watch the full pattern, not just whether a prescription exists. If focus improves, routines stabilize, cravings drop, and therapy participation gets stronger, treatment is likely helping. If sleep falls apart, mood gets erratic, or the person starts obsessing over pills, the plan needs review.
What should families watch for if misuse is a concern
Families should watch for behavior that suggests the medication is no longer being used as prescribed.
Common warning signs include:
- Running out early, which may point to overuse, sharing, or dose escalation
- Secrecy, including hidden bottles, changing stories, or anger when basic questions are asked
- Using the medication for a purpose other than ADHD, such as partying longer, counteracting a crash, or getting through withdrawal
- Sudden instability, including insomnia, irritability, appetite loss, or unusually reckless behavior
Families do not need proof before asking for help. A concerning pattern is enough reason to request a medication review.
What is the first step if someone in Dallas needs help now
Start with a full assessment that looks at ADHD symptoms and substance use at the same time. In Dallas, that means asking practical questions first. What substances are involved right now? Is there a withdrawal risk? What medications is the person already taking? Are the biggest problems attention, cravings, sleep, mood, safety, or all of the above?
Good care starts with a clear picture. Guessing between stimulant and non stimulant adhd medication without checking for active addiction, withdrawal, or misuse history creates unnecessary risk.
If ADHD symptoms and substance use are colliding, help is available now through Tru Dallas Detox & Recovery Center. The team serves Dallas-Fort Worth from a modern Euless facility and provides medically supervised detox, dual diagnosis treatment, medication-assisted treatment, and ongoing recovery planning. Reach out to discuss symptoms, verify PPO insurance, or get confidential guidance on the safest next step for you or your family.