When you’re struggling with both addiction and a mental health condition, treating them separately just doesn't work. It’s like trying to put out two fires in the same house by only focusing on one room. Lasting recovery means healing the whole person, which is exactly what dual diagnosis treatment programs are designed to do.
Key Takeaways
- Dual diagnosis is when a substance use disorder and a mental health condition happen at the same time.
- These conditions create a reinforcing cycle, with one making the other worse.
- Treating only the addiction or only the mental health issue is a primary cause of relapse.
- Integrated treatment that addresses both disorders simultaneously is essential for lasting recovery.
- The goal is to heal the whole person, not just treat isolated symptoms.
What Happens When Addiction and Mental Health Collide
Imagine trying to fix a car's engine without ever checking the electrical system. You might get it running for a while, but if the real problem is faulty wiring, you're guaranteed another breakdown. This is the perfect way to think about treating addiction without also addressing mental health. When these two issues exist together—a condition we call dual diagnosis or co-occurring disorders—they create a tangled, destructive cycle that’s incredibly hard to escape on your own.
It often starts with self-medication. Someone battling anxiety, depression, or past trauma might turn to substances for temporary relief. But over time, that substance use almost always makes the original mental health symptoms worse. This kicks off a feedback loop where each condition feeds the other, making recovery feel impossible.
The Cycle of Co-Occurring Disorders
The link between substance use and mental health isn't a one-way street. The connection is deeply intertwined, which is why a specialized, integrated approach is so vital.
- Self-Medication: An individual with intense social anxiety might start drinking to feel more comfortable in social situations, eventually leading to alcohol dependence.
- Worsening Symptoms: Chronic substance use can physically alter brain chemistry, which can trigger or intensify underlying mental health disorders like depression or bipolar disorder.
- Barriers to Healing: If you only treat the addiction, the unresolved mental health issue remains a powerful, constant trigger for relapse.
The medical community has woken up to this reality in a big way. A global analysis of research trends shows a massive spike in dual diagnosis studies since the mid-1990s, with the U.S. contributing over 62% of all publications. This scientific focus confirms what we see every day: people with a dual diagnosis face more severe symptoms, higher relapse rates, and poorer outcomes when their conditions aren't treated together. Learn more about these important research findings.
Why Integrated Treatment Is the Only Way Forward
Treating co-occurring disorders at the same time isn’t just a good idea—it’s the evidence-based gold standard for real, lasting recovery. An integrated plan accepts that you can't untangle one issue without working on the other. If you'd like to dive deeper, you can explore our article on how addiction affects mental health.
Effective dual diagnosis treatment programs bring together therapists, medical doctors, and counselors to create one unified strategy. This approach finally breaks the cycle by giving you the tools to manage both your mental health and your sobriety, paving the way for a stable, healthier future.
Building a Foundation for Recovery with Medical Detox
Before you can even begin to tackle the deeper emotional and psychological work of recovery, your body and mind need to be on solid ground. For anyone walking into a dual diagnosis treatment program, that solid ground is built during a medically supervised detox. Think of it as the non-negotiable first step—it creates the stability you need for real, lasting healing to begin.
Trying to detox on your own is risky enough, but when you add a co-occurring mental health condition to the mix, it becomes downright dangerous. The withdrawal process is already tough, but a mental health disorder can amplify and complicate every single symptom in unpredictable ways.
Why Professional Detox Is Critical for Dual Diagnosis
Withdrawal from substances like alcohol or opioids is a physically brutal experience on its own. Now, imagine piling a full-blown panic attack, a crushing depressive episode, or intense paranoia right on top of that. That’s the reality for someone with a dual diagnosis.
A mental health condition can turn the distress of withdrawal up to an eleven. For example, the baseline anxiety that comes with alcohol withdrawal can feel completely unbearable for someone who already struggles with a panic disorder. Without professional help, that overwhelming feeling often drives a person right back to using, just to make the physical and emotional pain stop.
This is exactly where medical detox makes all the difference. It provides a safe, controlled, and compassionate environment where a clinical team can manage both sets of symptoms at the same time. This integrated approach not only keeps you safe but dramatically increases the odds of getting through detox successfully. If you’re just starting to look at your options, understanding what is medical detox is a great place to start.
What Happens During Medical Detox
During medical detox, you’re not left alone to "tough it out." A dedicated clinical team provides 24/7 care to manage both the physical agony of withdrawal and the psychological storm of a flaring mental health condition. It’s a precise medical process from start to finish.
- Symptom Management: Doctors can provide medications to ease withdrawal symptoms like nausea, tremors, and insomnia, while also addressing psychiatric symptoms like severe anxiety or mood swings.
- Constant Monitoring: Your vital signs are checked around the clock to prevent dangerous complications, such as seizures or delirium tremens (DTs), which can be life-threatening.
- Emotional Support: You’ll have therapists and counselors right there with you, helping you navigate the fear, anxiety, and emotional chaos that often comes with detox.
Ultimately, this process is about so much more than just getting through withdrawal. It’s about creating the calm and clarity needed for the real work of recovery to begin. By stabilizing your body and mind, medical detox lays the foundation upon which a new, healthier life can be built.
Finding Your Place on the Path to Healing
Recovery isn’t a one-size-fits-all process. The environment where you heal plays a huge role, and because everyone's journey is unique, the best dual diagnosis treatment programs provide a full spectrum of care. Think of it as a pathway with different levels of support, designed to meet you exactly where you are and evolve with you as you get stronger.
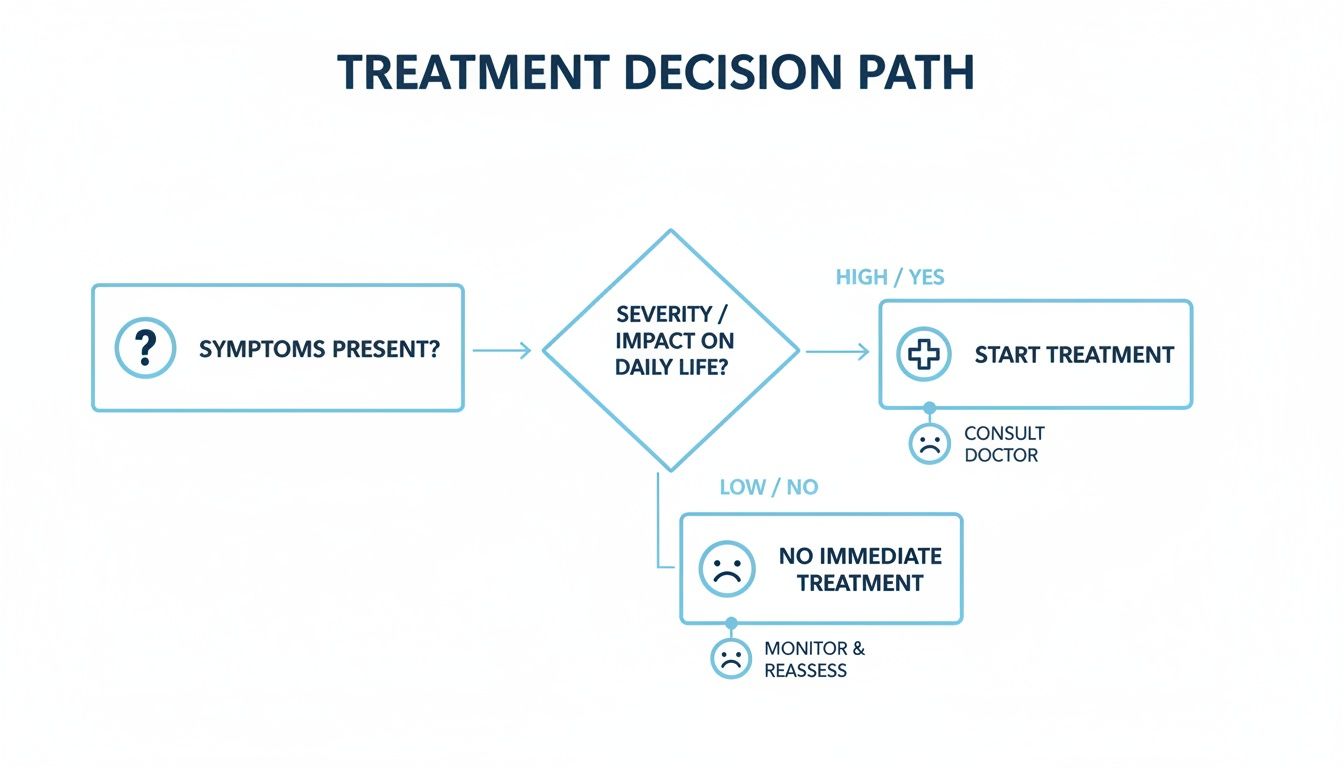
The first step, and often the hardest, is simply deciding to start. This decision tree helps put that powerful choice into perspective.
This visual gets to the heart of it: every single recovery story begins with the moment someone recognizes they need help and says "yes" to treatment.
To really get a feel for the different levels of care, let's use an analogy. Imagine you're learning to swim. Each stage of treatment provides a specific type of support, just like a swim instructor would adjust their approach based on your confidence in the water.
Inpatient or Residential Treatment: The Deep End with an Instructor
Inpatient treatment is the most immersive, hands-on level of care you can get. It’s like having an instructor in the deep end with you 24/7. You live at the facility, which removes you from the daily triggers and stresses that might fuel substance use or mental health symptoms. Your only job is to focus on getting well.
This kind of highly structured setting is a lifeline for anyone who is medically unstable, faces a high risk of relapse, or simply doesn't have a safe, supportive home to return to. Days are packed with a schedule of individual and group therapy, medical care, and other healing activities, giving you a constant safety net during the most fragile phase of early recovery.
Partial Hospitalization Programs (PHP): Intensive Lessons from the Poolside
A Partial Hospitalization Program, or PHP, is the next step down. Sticking with our swimming analogy, this is like taking intensive lessons every day with an instructor coaching you from the edge of the pool. You’ve got the basics down and can stay afloat, but you still need that daily, structured guidance to build your strength and technique.
With a PHP, you’ll spend a significant portion of your day at the treatment center—usually five to seven days a week—but you go home or to a sober living house at night. This setup strikes a great balance between intensive support and growing independence, making it a perfect transition for those leaving inpatient care or for people who have a stable home life but still need daily therapeutic structure.
Intensive Outpatient Programs (IOP): Weekly Coaching to Refine Your Stroke
An Intensive Outpatient Program (IOP) offers another step toward independence. Now, you’re like a swimmer who meets with a coach a few times a week to refine your stroke and build endurance. You’re navigating the water on your own for the most part, but that consistent, professional guidance keeps you sharp and on track.
IOPs typically require you to attend therapy for a few hours at a time, maybe three to five days a week. This level of care is built for people who have already developed solid coping skills and are ready to jump back into their lives—whether that’s work, school, or family. It gives you the chance to apply what you’ve learned in the real world while still having a team to fall back on.
Understanding the differences between these levels of care is crucial when deciding on a treatment path. The table below breaks down the key features of each program to give you a clearer picture.
Comparing Levels of Care for Dual Diagnosis Treatment
| Feature | Inpatient/Residential | Partial Hospitalization (PHP) | Intensive Outpatient (IOP) |
|---|---|---|---|
| Living Situation | Reside at the facility 24/7 | Live at home or sober living | Live at home or sober living |
| Time Commitment | Full-time, 24 hours a day | 5-7 days/week, 4-6 hours/day | 3-5 days/week, 3-4 hours/day |
| Level of Supervision | Constant medical and clinical supervision | High level of clinical structure during program hours | Moderate clinical support and accountability |
| Best For | Medical/psychological instability, high relapse risk, unsupportive environment | Transitioning from inpatient, stable home life but needs daily structure | Strong coping skills, integrating back into work/school/family |
| Focus | Stabilization, detox, and intensive foundational therapy | Building skills, structured accountability, and gradual autonomy | Real-world application of skills, maintaining recovery, and community reintegration |
Ultimately, the goal is to find a program that provides the right amount of support for your current needs, with the flexibility to adapt as you progress.
The ability to move seamlessly between these levels of care is a hallmark of high-quality dual diagnosis treatment programs. This "continuum of care" ensures that you are never left without the right support. As you gain strength, you can step down to a less intensive level without losing the connection to your therapeutic team.
This gradual progression is so important. It helps you avoid the shock of going from a completely sheltered environment straight back into the complexities of daily life—a common trigger for relapse. By slowly taking on more responsibility while keeping that clinical safety net in place, you build a much stronger foundation for lasting wellness.
The Therapeutic Toolkit for Integrated Recovery
So, what does integrated treatment actually look like day-to-day inside a dual diagnosis treatment program? It's a lot more than just talking. It’s about using a specific set of powerful, evidence-based tools designed to heal both the addiction and the mental health disorder at the same time. This whole approach is built on a simple but critical idea: both conditions need to be addressed with equal intensity and expertise.
Think of it like being a skilled carpenter. You wouldn’t try to build a sturdy house with just a hammer. You’d need a full toolkit—saws, drills, levels, and measuring tapes—each with a specific job. In integrated recovery, our "tools" are different therapeutic methods, each designed to tackle a different part of the healing process.
Rewiring the Brain with Behavioral Therapies
At the very core of dual diagnosis treatment are behavioral therapies. These are designed to help you understand and change the destructive thought patterns that fuel both addiction and mental illness. We're not just trying to manage symptoms here; the real goal is to rewire your brain for healthier responses.
Two of the most effective therapies you'll encounter are:
- Cognitive Behavioral Therapy (CBT): This is a cornerstone of modern therapy. CBT helps you identify, challenge, and ultimately reframe the negative thinking that leads to harmful behaviors. For someone with social anxiety and an alcohol use disorder, CBT helps them recognize a thought like, "I need a drink to talk to people," and replace it with something healthier and more realistic. You can learn more about how this works by reading our guide on CBT for addiction.
- Dialectical Behavior Therapy (DBT): Originally developed for borderline personality disorder, DBT has become a powerhouse in dual diagnosis care because it's brilliant at teaching emotional regulation. It gives you practical skills in mindfulness, distress tolerance, and interpersonal effectiveness—all crucial for managing intense emotions without turning to substances.
Processing the Past to Heal the Present
More often than you’d think, unresolved trauma is the hidden engine driving both substance use and mental health conditions. That's why therapies designed to process these deep-seated wounds are absolutely essential for so many people in recovery.
Eye Movement Desensitization and Reprocessing (EMDR) is a highly structured therapy that helps the brain finally process traumatic memories. For someone with PTSD who uses substances to numb flashbacks, EMDR can significantly reduce the emotional charge of those memories, removing a major trigger for relapse.
Stabilizing Brain Chemistry with Medication
Sometimes, therapy alone isn't enough, especially in the early stages of recovery. Your brain chemistry might be so off-kilter from substance use and mental illness that it's tough to even engage in the therapeutic process. This is where Medication-Assisted Treatment (MAT) can be a real game-changer.
MAT uses specific, FDA-approved medications to reduce cravings, manage withdrawal symptoms, and stabilize brain function. This isn't about replacing one drug with another. It's about using medicine as a tool to create the mental space and stability needed for therapy to truly take root and be effective.
For instance, medications like naltrexone can help curb alcohol cravings, while buprenorphine is used to manage opioid withdrawal. This medical support provides a crucial foundation, allowing you to focus your energy on the deep psychological work recovery requires.
The Power of Combined and Holistic Approaches
The most effective dual diagnosis treatment programs don't just rely on one or two of these tools. They create a personalized plan that weaves clinical therapies together with holistic practices that heal the whole person—mind, body, and spirit.
This often includes:
- Group Therapy: Finding a community of people who actually get it is incredibly healing.
- Family Therapy: Healing the family system is key to building a strong support network for when you return home.
- Mindfulness and Meditation: Learning to stay grounded in the present moment can be a superpower for managing stress.
- Nutritional Counseling: Helping your body recover is just as important as helping your mind.
This integrated approach gets powerful results. Statistics show that 85-95% of individuals who complete rehab remain drug-free nine months later, with 80% reporting a significant improvement in their quality of life. The use of MAT is a major factor here, with 39% of U.S. facilities providing these medications for alcohol use disorder. However, with relapse rates for chronic diseases hovering around 40-60%, it's clear that ongoing, integrated care is vital for long-term wellness.
How to Choose a High-Quality Treatment Program
Let's be honest: not all treatment centers are the same, especially when you're dealing with co-occurring disorders. Finding the right dual diagnosis treatment program is more than just a quick search online. It’s a deliberate choice that can set the entire foundation for a lasting recovery. The real goal is to find a center that offers truly integrated care, not just two separate programs that happen to be in the same building.
This isn't a niche problem anymore. The demand for quality dual diagnosis care is surging, with the global market projected to hit $12.6 billion by 2033. That growth is a direct response to a very real need—somewhere around 50-60% of people with a substance use disorder also have a co-occurring mental health condition. This isn't just a statistic; it's a reality that demands specialized, expert care. You can get a deeper look at this market trend over at HTF Market Insights.
So, how do you cut through the noise and find a program that’s actually built for healing? It comes down to knowing what to look for and what questions to ask.
Verifying Credentials and Philosophy
Before you even think about therapies or amenities, you have to confirm a program's legitimacy and core beliefs. Great care starts with a solid foundation of professional expertise and a clear, unified philosophy that puts integrated recovery first, right from day one.
Start with these absolute must-haves:
- Licensing and Accreditation: Is the facility licensed by the state? Is it accredited by a reputable organization like The Joint Commission or CARF? This isn't just paperwork; it’s your proof that they meet strict national standards for safety and quality.
- Staff Credentials: The clinical team should be made up of licensed professionals who have real-world experience with dual diagnosis. You want to see medical doctors, psychiatrists, licensed therapists (LPCs, LCSWs), and certified addiction counselors on the team.
- A Genuinely Integrated Model: This is the big one. Ask them point-blank: "How do you integrate mental health and substance use treatment?" A top-tier program won't just pass you between departments. They'll have one cohesive treatment plan, with clinical teams that meet and collaborate every single day.
A truly integrated program means the psychiatrist treating your anxiety is in constant communication with the therapist leading your addiction group. This unified approach is the antidote to the fragmented care that so often leads to relapse.
Asking the Right Questions About Treatment
Once you've confirmed a program is credible, it's time to get into the details of how they actually help people. The answers to these questions will tell you everything you need to know about whether their services are right for you or your loved one.
Zero in on these key areas:
- Evidence-Based Therapies: Do they use proven methods like Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), or EMDR? These aren't just buzzwords; they are the gold standards for treating both addiction and mental health challenges at the same time.
- Continuum of Care: Can you transition smoothly from medical detox to inpatient care, and then step down to outpatient services with the same core team? A seamless continuum of care is critical for building trust and ensuring you have consistent support as you move forward.
- Family Involvement: How does the program bring family into the process? Addiction and mental illness affect the entire family, and programs that include loved ones in therapy and education see much better long-term outcomes.
- Aftercare Planning: What’s the plan for when you leave? A strong aftercare strategy—including alumni groups, connections to sober living, and referrals for ongoing therapy—shows that a center is invested in your lifelong well-being, not just your time in their program.
Making this decision can feel overwhelming, but arming yourself with the right questions helps you find a program that doesn't just treat symptoms—it heals the whole person.
Putting It All Together: Your Blueprint for Real Recovery
We've covered a lot of ground, from the first steps of detox to the deeper work of therapy. When you strip it all down, a handful of core ideas are what truly make dual diagnosis treatment work. Think of these as the essential pillars holding up your recovery journey. Keeping them front and center will help you navigate the process, ask the right questions, and build a future you can be proud of.
These aren't just nice-to-haves; they are the non-negotiables. The best dual diagnosis treatment programs are built on these principles, giving people the strongest possible foundation for getting—and staying—well.
The Bottom Line on Dual Diagnosis Care
Here’s what really matters when you're looking for help:
- Treat Everything at Once: Lasting recovery isn't possible if you treat addiction and a mental health condition as two separate issues. They have to be addressed together, at the same time, by the same team.
- Detox Safely: Starting with a medically supervised detox is the only safe way to begin. It stabilizes you physically and mentally, clearing the way for the real healing to start.
- Match the Care to Your Needs: Recovery isn't a straight line. A good program offers a full spectrum of care—from inpatient to outpatient—so you get the right amount of support exactly when you need it.
- Use Every Tool in the Toolbox: There's no single magic bullet. The most effective programs combine proven therapies like CBT and DBT with practical support like MAT to give you a well-rounded set of skills for life.
- Vet the Program and the People: Don't take a center's claims at face value. Look for official accreditation and make sure their team is truly experienced in integrated treatment, not just saying they are.
Frequently Asked Questions
What is the single most important factor in a dual diagnosis program?
If you have to boil it down to one thing, it’s a genuinely integrated approach. This means the therapists, doctors, and staff all see your substance use and mental health as two sides of the same coin. You get one treatment plan, not two separate ones, from the very beginning.
How do I know when I'm ready to move to a lower level of care?
That's never a decision you have to make alone. It’s a conversation between you and your treatment team. They’ll look at your progress, how you’re using your new coping skills, and the stability of your home environment to figure out the right time to transition to more independence. The goal is always a smooth handoff, not a sudden drop-off.
How can I tell if I have a dual diagnosis?
This is a tough one to figure out on your own. Often, the lines between mental health symptoms and substance use get incredibly blurred. You might notice you’re drinking to quiet your anxiety or using drugs to numb feelings of depression. The only way to know for certain is to get a professional assessment from a qualified clinical team who can see the full picture.
Will my insurance cover a dual diagnosis treatment program?
For the vast majority of people, the answer is yes. Most major health insurance plans are required to cover mental health and substance use treatment. Since integrated treatment is the evidence-based gold standard, it is considered a medical necessity. The easiest way to find out for sure is to call a treatment center's admissions team for a free, confidential check of your benefits.
What happens after I finish the program?
Recovery is a long-term process, and a good treatment program prepares you for it. A solid aftercare plan is a core part of the process and typically includes connections to alumni groups, referrals for ongoing therapy and support groups, and recommendations for sober living options to help you transition back to your life with confidence.