A person in Dallas often reaches this point after a night without sleep, a frightening crash, a call from family, or a moment of clarity that feels fragile. Someone searches for answers because quitting methamphetamine sounds necessary, but the unknown feels dangerous.
That fear is justified. Meth withdrawal can be intense, emotionally destabilizing, and hard to manage alone. It can also be managed safely with the right support, a realistic plan, and a clear understanding of what the methamphetamine recovery timeline usually looks like.
Families across Dallas, Euless, Irving, Arlington, and the wider DFW area often need practical guidance more than slogans. They need to know when symptoms start, when relapse risk rises, what kind of care fits each stage, and how to move from detox into real recovery. Emotional support matters too, especially when anxiety, shame, or depression are part of the picture, which is why some people also benefit from outside resources focused on counselling for emotional well-being alongside addiction treatment.
Table of Contents
- Starting Your Methamphetamine Recovery Journey in Dallas
- The First 72 Hours The Acute Withdrawal Crash
- Navigating the Full Methamphetamine Withdrawal Timeline
- Beyond the Crash Understanding Protracted Withdrawal PAWS
- Your Path to Recovery Evidence-Based Treatment in Dallas
- Building a Life After Meth Relapse Prevention Strategies
- When and How to Get Help at Tru Dallas Detox
Starting Your Methamphetamine Recovery Journey in Dallas
Stopping methamphetamine use often begins in a state of exhaustion and confusion. The person using may feel trapped between wanting help and dreading what happens next. Loved ones may be watching sleep patterns collapse, mood swings worsen, or paranoia show up, and they may not know whether to wait, intervene, or get professional support right away.
The clearest answer is this. Recovery is possible, but trying to force it through willpower alone usually creates more risk than progress. A realistic methamphetamine recovery timeline includes detox, stabilization, ongoing therapy, and relapse prevention. It isn't just about getting through a few bad days.
In Dallas, that matters because access to treatment can change the outcome quickly. A local detox center can reduce the delay between deciding to stop and entering care. That gap is often where people return to use, not because they don't want recovery, but because the symptoms become overwhelming before support is in place.
What people usually need at the beginning
Early recovery works better when a few basics are handled immediately:
- Safe monitoring: Severe fatigue, depression, agitation, and confusion can shift quickly in the first days.
- A simple next step: People do better when they know where to go and what admission looks like.
- Mental health screening: Meth use and emotional distress often overlap, and treatment should address both.
- A plan beyond detox: Detox helps start recovery. It doesn't complete it.
Clinical reality: The beginning of recovery often feels chaotic. Good treatment makes the process structured, predictable, and safer.
For many people in North Texas, the most helpful approach is local, medically supervised care that removes access to the drug, lowers immediate relapse risk, and creates a path into continued treatment. That gives families in neighborhoods from Oak Cliff to North Dallas a practical way to act instead of waiting for another crisis.
The First 72 Hours The Acute Withdrawal Crash
The first part of the methamphetamine recovery timeline is often the hardest to predict emotionally, even when the physical pattern is familiar. Methamphetamine pushes the brain far past its normal reward and alertness settings. When use stops, the person doesn't just feel tired. The system drops hard.
A useful way to understand this is dopamine debt. During active use, the brain is driven into an artificial state of energy, focus, and reward. When the drug is removed, that borrowed stimulation has to be repaid. The result is the crash.
Why the crash feels so severe
The crash typically begins within 24 to 48 hours of the last use and is marked by severe fatigue, depression, and hypersomnia, according to meth withdrawal clinical guidance. During this period, cravings are the most reported symptom in 95% of cases and can persist for up to 7 weeks, which is one reason early detox support matters so much.
People often expect agitation only. Instead, many sleep heavily, feel emotionally flat or severely hopeless, and have almost no ability to manage stress. Some also experience paranoia or hallucinations. Appetite may return sharply after periods of poor nutrition.
A person trying to do this alone in an apartment, hotel room, or family home in Dallas can change course quickly. One hour may look like exhaustion. The next may look like panic, desperation, or a sudden decision to use again just to make the symptoms stop.
What usually helps in a Dallas detox setting
A supervised detox setting doesn't make withdrawal disappear. It does make the process safer and more manageable.
- Observation through the crash: Staff can respond when depression deepens, thinking becomes disorganized, or psychiatric symptoms appear.
- Support for basic functioning: Hydration, food, rest, and calm structure matter more than many people expect.
- Protection from immediate relapse: The highest-risk window is often the period when cravings are intense and judgment is poor.
- Transition planning: Detox should lead directly into further treatment, not into an unstructured discharge.
People who want a more detailed overview of symptom patterns can review this guide on meth withdrawal symptoms and detox.
A meth crash isn't laziness, weakness, or lack of motivation. It's a withdrawal state that can leave the person too depleted to think clearly.
For families in DFW, this is usually the point to stop negotiating with the problem and start arranging care.
Navigating the Full Methamphetamine Withdrawal Timeline
The first crash doesn't define the whole methamphetamine recovery timeline. What follows is usually a shifting pattern of fatigue, cravings, mood symptoms, and cognitive fog. People often mistake this variability for failure. It isn't. It's the brain and body trying to stabilize after repeated stimulant exposure.
Clinical research describes methamphetamine withdrawal as an acute phase lasting 7 to 10 days and a subacute phase lasting at least 2 additional weeks, with cravings remaining the most persistent symptom and relapse risk peaking on days 3 to 5 as energy returns before impulse control fully recovers, according to this PubMed summary of methamphetamine withdrawal.
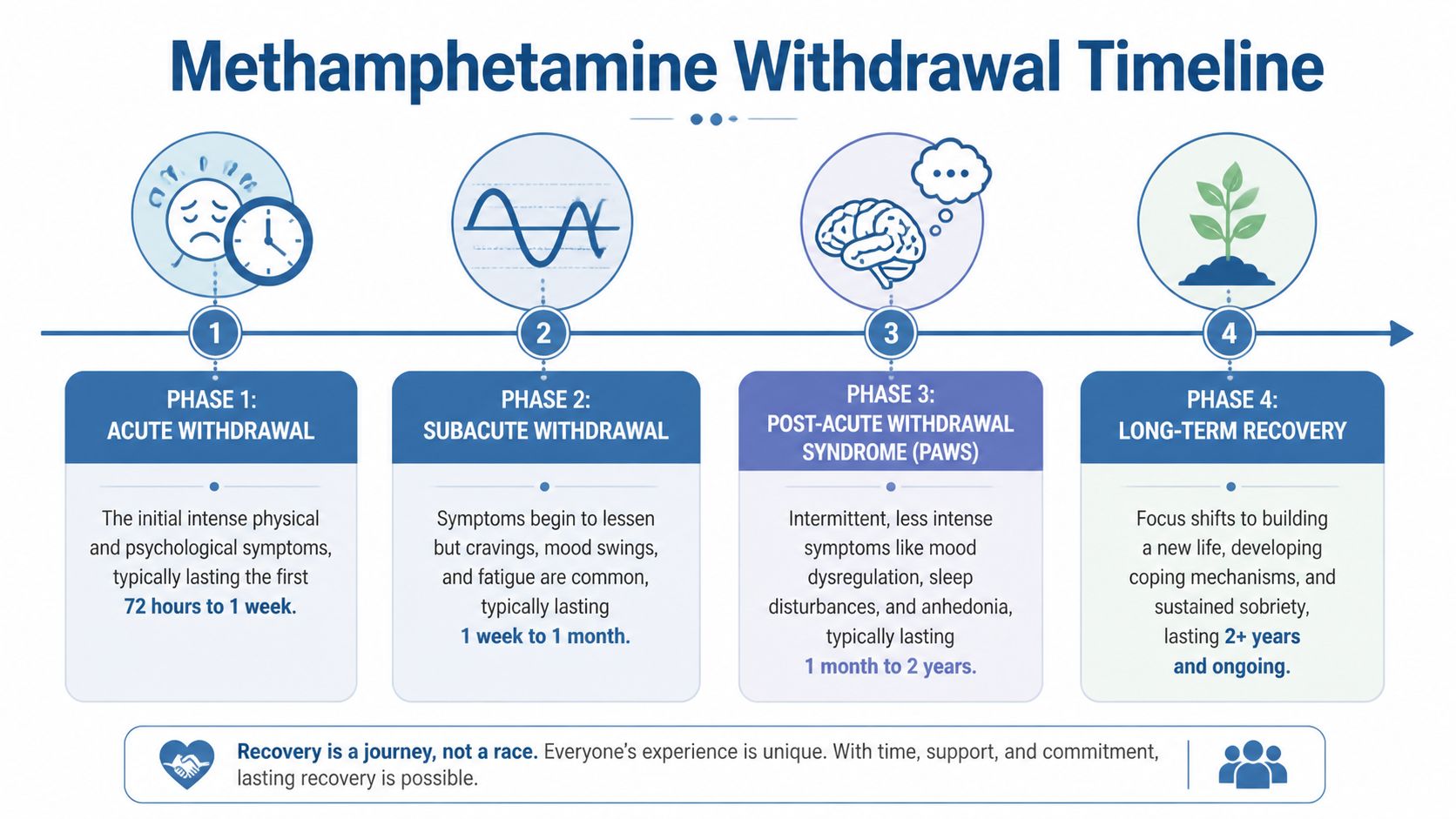
Methamphetamine recovery timeline at a glance
| Phase | Typical Duration | Common Symptoms | Focus of Support |
|---|---|---|---|
| Crash phase | First 24 to 48 hours | Severe fatigue, depression, hypersomnia, appetite rebound, emotional instability | Safety, rest, nutrition, observation |
| Acute withdrawal | About 7 to 10 days | Dysphoria, anxiety, agitation, low motivation, cognitive fog, ongoing cravings | Medical monitoring, structure, sleep support, therapy engagement |
| Subacute withdrawal | At least 2 more weeks | Lower-level but persistent symptoms, mood fluctuation, irritability, poor concentration | Consistency, counseling, trigger management, daily routine |
| Protracted recovery | Weeks to months or longer | Intermittent cravings, sleep disruption, emotional flatness, stress sensitivity | Relapse prevention, mental health care, outpatient support, sober network |
Why one timeline can look different from another
No two people in Dallas will move through this timeline in exactly the same way. The duration and intensity can shift based on patterns of use, how long methamphetamine has been used, whether other substances are involved, and whether depression, anxiety, or other psychiatric conditions are also present.
That last point matters. When mental health symptoms are already in the picture, withdrawal can feel more complicated and more discouraging. A person may interpret low motivation as a character problem when it's part of recovery and needs treatment, not criticism.
A more useful question than "How long until this is over?" is "What support matches the current phase?"
- Early days need containment: Sleep, food, safety, and professional observation.
- The next stretch needs structure: Regular schedule, therapy, reduced exposure to triggers.
- Later recovery needs repetition: Skills practice, accountability, and support when symptoms come in waves.
Practical rule: Recovery usually improves when care intensity matches symptom intensity. The mistake isn't needing help. The mistake is stepping down too early.
For many people in the Dallas area, the timeline gets easier to manage once it stops being a mystery.
Beyond the Crash Understanding Protracted Withdrawal PAWS
One of the most frustrating parts of the methamphetamine recovery timeline happens after the worst of detox seems over. The person may expect to feel normal once the acute withdrawal phase passes. Instead, motivation may stay low, sleep may remain irregular, and pleasure may feel muted. That doesn't mean recovery has stalled.
What PAWS really means
Protracted withdrawal, often called PAWS, is the longer healing period that can follow early withdrawal. A simple way to understand it is brain rewiring. Methamphetamine has pushed reward, attention, and stress systems into unhealthy patterns. Those systems don't reset on command.
PAWS can look like:
- Mood swings: A person may feel stable one day and discouraged the next.
- Low energy: Not the same crash as detox, but a persistent sense of being drained.
- Anhedonia: Everyday life doesn't feel rewarding yet.
- Sleep disruption: Some people sleep too much. Others sleep poorly.
- Craving flare-ups: Triggers can reactivate strong urges even after a period of improvement.
This stage often creates shame because symptoms are less dramatic than detox but more confusing. Families may say, "You should be better by now." That kind of pressure usually backfires.
The absence of a dramatic crisis doesn't mean the brain has finished healing.
What support looks like during this stage
PAWS responds poorly to isolation and guesswork. It responds better to ongoing treatment, predictable routine, and mental health support. In the Dallas-Fort Worth area, that often means stepping into outpatient care, therapy, support groups, or continued psychiatric follow-up after detox or residential treatment.
Useful supports during this stage often include:
- Therapy for triggers and thought patterns: Especially when cravings are linked to stress, shame, or old routines.
- Sleep and routine work: Wake time, meals, movement, and bedtime consistency help stabilize recovery.
- Dual diagnosis care: If depression or anxiety continue, they should be treated directly.
- Family education: Loved ones need to understand that emotional flatness isn't defiance.
PAWS isn't a sign that treatment failed. It's often a sign that recovery has moved into the longer, less visible work of rebuilding daily life.
Your Path to Recovery Evidence-Based Treatment in Dallas
The methamphetamine recovery timeline becomes safer and more manageable when treatment matches the stage of recovery. People usually struggle most when they try to compress the whole process into one decision. Detox alone isn't enough. At the same time, skipping detox when symptoms are severe can create unnecessary risk.
Detox, residential care, and outpatient support
A solid treatment path usually works in layers.
Detox handles the immediate withdrawal period. During this period, medical monitoring, psychiatric observation, nutrition, rest, and stabilization matter most. For someone dealing with severe exhaustion, depression, paranoia, or strong cravings, detox creates a buffer between stopping meth and returning to use.
Residential treatment helps after the body is more stable but the mind is still vulnerable. This level of care is useful when the home environment is chaotic, triggers are everywhere, or the person has a pattern of leaving treatment too early. It gives recovery enough time to become more than a short-term emergency response.
Outpatient care helps when the person is stable enough to live at home or transition back to daily responsibilities while continuing treatment. This is often where relapse prevention skills get tested in real life.
One local option is methamphetamine rehab in Dallas, which outlines how detox and continued treatment can be linked rather than treated as separate problems.
What to look for in a Dallas treatment program
Families searching for addiction treatment in Dallas often focus on admission speed first. That's understandable, but quality of care still matters. A program should fit the actual risks of meth withdrawal and the longer recovery process that follows.
Key features to look for include:
- 24/7 clinical monitoring during detox: Early symptoms can shift quickly.
- Dual diagnosis capability: Meth use and mental health symptoms often overlap.
- A clear step-down plan: Detox should connect to residential or outpatient treatment, not end in uncertainty.
- Individualized care planning: The right timeline is personalized, not generic.
- Family communication and discharge planning: Recovery improves when home expectations are realistic.
Tru Dallas Detox & Recovery Center provides medically supervised detox, dual diagnosis treatment, and continued levels of care from its Euless location serving the Dallas-Fort Worth area.
The practical trade-off is simple. Quitting alone may feel faster and more private, but it usually leaves the person exposed during the most unstable points of withdrawal and early recovery. Structured care asks for more commitment up front, but it gives the recovery process a real framework.
Building a Life After Meth Relapse Prevention Strategies
Relapse prevention isn't a separate topic from the methamphetamine recovery timeline. It's part of it from the beginning. Meth changes reward, stress response, and decision-making in ways that make early recovery fragile. That reality should be faced directly, not softened.
According to meth relapse data, up to 93% of individuals addicted to methamphetamine relapse, and for those trying to recover without professional help, the long-term success rate after three years is 5%. Those numbers don't mean recovery is hopeless. They mean the plan has to be stronger than good intentions.
Why relapse prevention has to be planned early
People relapse for different immediate reasons, but the pattern is often familiar. They leave detox feeling determined. Then sleep stays off, stress returns, motivation drops, old contacts reappear, and cravings hit harder than expected. Without a structured response, relapse can start looking like relief.
A better approach is to assume that pressure points will come and plan for them before they do.
Recovery works better when the person expects triggers and rehearses a response, instead of assuming motivation alone will carry the week.
Practical strategies that support long-term recovery
Some approaches tend to hold up better over time than others:
- Identify high-risk triggers: Specific people, neighborhoods, payday patterns, arguments, and isolation periods should be named clearly.
- Use behavioral therapy: CBT can help a person catch the thought pattern that usually comes before a return to use.
- Build sober support on purpose: Recovery isn't strengthened by vague promises to "stay busy." It improves with regular contact, meetings, therapy, and accountability.
- Create a discharge routine: Wake time, meals, transportation, appointments, and emergency contacts should be decided before treatment ends.
- Address language and communication barriers when needed: Some families respond better when counseling is accessible in the language they use at home. In those cases, resources like multilingual addiction recovery therapy can make support easier to engage with consistently.
What usually doesn't work is relying on shame, isolation, or a single promise that "this time is different." Sustainable recovery is built through repetition, structure, and support that continues after the crisis has passed.
When and How to Get Help at Tru Dallas Detox
People often wait for one more disaster before reaching out. Another binge. Another psychotic episode. Another disappearance. Another promise to quit tomorrow. With methamphetamine, that delay can make the first stage of recovery harder and more dangerous than it needs to be.
Signs it is time to reach out now
The time to seek help is now if any of these are happening:
- The crash is already starting: Severe exhaustion, depression, or confusion after stopping use.
- Psychiatric symptoms are showing up: Paranoia, hallucinations, panic, or disorganized thinking.
- Relapse keeps happening quickly: The person can't get past the first days without returning to meth.
- Home isn't a safe recovery setting: Drug access, conflict, or no reliable support.
- Mental health concerns are mixed in: Depression, anxiety, or emotional instability are complicating recovery.
For people who want to understand what supervised admission involves, this overview of medically supervised detox in Dallas can help make the first call feel less intimidating.
The first step is simple
The first step isn't committing to every future stage of treatment today. It's getting evaluated, asking questions, and finding out what level of care fits the current situation. That may mean detox first. It may mean planning for residential or outpatient treatment next. What matters most is breaking the cycle of trying to manage a serious stimulant withdrawal process alone.
For families in Dallas, Plano, Irving, Garland, Arlington, and nearby communities, quick action often matters more than perfect timing. Help is most useful when symptoms are active, motivation is present, and a safe transition can happen before the next relapse.
If methamphetamine use is disrupting life, relationships, sleep, or mental health, reach out to Tru Dallas Detox & Recovery Center for confidential help. A clinical team can answer questions, discuss treatment options, and help with next steps such as admissions and insurance verification. The safest time to ask for help is before the next crash, not after it.