Some readers arrive at this moment confused by a strange contradiction. They stopped drinking because alcohol was draining their life, yet now they can barely get out of bed. They may feel shaky, restless, sweaty, and completely worn out at the same time.
That reaction is frightening, but it isn’t a character flaw and it isn’t laziness. In alcohol withdrawal and tiredness often show up together because the brain, nervous system, sleep cycle, and the rest of the body are all trying to rebalance at once. A person can feel wired and exhausted in the same hour.
For families across Dallas, Highland Park, Oak Lawn, Plano, Irving, Arlington, and the wider DFW area, this is one of the most misunderstood parts of early recovery. Someone may look like they should sleep it off. In reality, alcohol withdrawal fatigue can be part of a medically serious process that deserves careful attention.
The good news is that this exhaustion has a clear medical explanation. It also follows patterns that can be recognized, supported, and treated safely. With the right help from a Dallas detox center, people don’t have to guess whether what they’re feeling is normal, dangerous, or a sign they’re failing. They can get real answers and a safer path forward.
Table of Contents
- The Overwhelming Exhaustion After Your Last Drink
- Why Your Body Feels So Tired During Alcohol Withdrawal
- The Timeline of Alcohol Withdrawal Fatigue From Days to Months
- Key Factors That Influence Withdrawal Severity
- Safe At-Home Strategies to Manage Mild Fatigue
- Why Medical Detox in Dallas is the Safest Path to Recovery
- Take the First Step Toward Renewed Energy in Dallas
- Frequently Asked Questions About Alcohol Withdrawal
The Overwhelming Exhaustion After Your Last Drink
Many people who stop drinking are caught off guard by the heaviness that follows. In Dallas, someone may decide to quit and brace for shaking, nausea, or a sleepless night. Then a different symptom takes center stage. Getting out of bed feels difficult. Walking to the kitchen feels strangely hard. The body is worn out, yet rest still does not come easily.
That combination can feel unsettling.
Alcohol withdrawal fatigue can be part of a medically serious process that deserves careful attention. It often feels less like ordinary tiredness and more like a full-system crash. Muscles may feel weak. Thoughts may seem slow or foggy. At the same time, the nervous system can stay keyed up, which leaves the person exhausted but unable to fully relax.
A simple comparison helps here. It works like a house after a power surge. Some circuits are overfiring while others are struggling to keep up. From the outside, the person may just look sleepy. Inside, the brain and body are working hard to regain balance.
Clinicians regularly see this pattern during detox. Fatigue is a physical symptom, not a sign of low motivation or poor character. For some people, it peaks early and starts to ease within days. For others, it comes in waves and lingers longer, especially if sleep, nutrition, anxiety, or depression have already been affected by alcohol use.
That longer arc matters. The exhaustion of early withdrawal is only part of the story. Some people later deal with post-acute withdrawal symptoms, often called PAWS, where low energy, poor concentration, and unrefreshing sleep continue after the most intense detox symptoms have passed. Generic articles often miss this connection, but it shapes treatment decisions in real life, especially for people trying to keep up with work, parenting, or family responsibilities across Dallas-Fort Worth.
This is one reason a dual-diagnosis approach can make such a difference. If fatigue is tied not only to withdrawal, but also to depression, trauma, anxiety, or another mental health condition, treatment needs to address both at the same time. A person may need medical detox for immediate safety, then follow-up care that supports sleep, mood, nutrition, and mental health recovery together. For a broader look at symptoms that can appear alongside this exhaustion, see our guide to alcohol detox side effects.
Clear answers reduce fear. The right level of care helps people get through the first crash, understand what may come next, and build a plan for recovery that matches the full timeline from acute withdrawal to possible PAWS.
Why Your Body Feels So Tired During Alcohol Withdrawal
Your brain is trying to rebalance
Alcohol changes how the brain controls calm and stimulation. With repeated drinking, the brain adjusts to alcohol being present. It reduces some of its natural calming activity and increases systems linked to alertness and stress. When alcohol is removed, those changes do not reverse in a day.
The result is a strained nervous system. A person can feel wired and worn out at the same time. That combination confuses people, but it is common in withdrawal.
One part of the story involves GABA and glutamate. GABA helps quiet brain activity. Glutamate helps activate it. Alcohol pushes that balance off center. During withdrawal, the brain often has too little braking and too much acceleration, which can lead to shakiness, anxiety, poor sleep, and deep fatigue.
Stress chemicals add another layer. Norepinephrine rises during withdrawal, and the body shifts into a fight-or-flight state. Muscles stay tense. Heart rate may rise. Thoughts may race. Even without much physical activity, the body is spending energy as if it needs to stay on guard.
That is why exhaustion during withdrawal does not feel like ordinary tiredness. It is closer to running a motor too hard while the fuel system is unstable.
For readers who want a broader view of the symptoms that can appear alongside fatigue, this guide to alcohol detox side effects can help put the whole picture together.
Sleep stops being restorative
Many people expect sleep to fix the problem. During withdrawal, sleep often loses its repair function for a while.
Alcohol disrupts normal sleep architecture. It can reduce healthy REM patterns, fragment deeper stages of sleep, and train the brain to rely on alcohol-related sedation instead of natural sleep signals. After the last drink, the brain has to rebuild a more normal rhythm. During that adjustment, a person may fall asleep late, wake often, dream intensely, or get up feeling as tired as before bed.
This mismatch is frustrating. The body asks for rest, but the nervous system keeps interrupting it.
In Dallas treatment settings, this matters because ongoing sleep disruption can blur the line between acute withdrawal fatigue and early post-acute symptoms. If someone also has anxiety, depression, trauma, or another mental health condition, poor sleep can keep draining energy long after the first detox window ends. That is one reason dual-diagnosis care matters. It treats the withdrawal process and the mental health drivers that can keep fatigue going.
The body is spending energy on repair
The brain is not the only system under strain. The rest of the body is also trying to recover.
Alcohol use can affect hydration, blood sugar regulation, appetite, vitamin levels, hormone balance, and inflammation. Once drinking stops, the body begins correcting those problems. That repair work takes energy. If someone has been eating poorly, vomiting, sweating heavily, or sleeping badly, the energy deficit can feel even sharper.
Small tasks may suddenly feel much harder than expected. Taking a shower, making breakfast, answering a work message, or driving across Dallas can feel like too much for the day.
A few patterns often show up together:
- Physical heaviness can make the arms and legs feel weighted down.
- Mental fog can slow concentration, memory, and decision-making.
- Emotional depletion can show up as irritability, flat mood, or feeling overwhelmed by ordinary demands.
- Restless exhaustion means feeling tired without being able to settle or rest effectively.
Some people also have an underlying medical or psychiatric issue that alcohol had been masking. Anemia, liver stress, dehydration, panic symptoms, and depression can all add to withdrawal fatigue. That is another reason a careful assessment matters, especially for people whose exhaustion feels extreme, lasts longer than expected, or comes with mood symptoms.
Practical rule: Severe tiredness with confusion, hallucinations, seizures, chest pain, fainting, or major changes in pulse, blood pressure, or breathing needs medical care right away.
Understanding the biology helps remove some of the fear. Fatigue during alcohol withdrawal usually means the brain and body are working hard to regain balance. In Dallas, the safest plans look at the full arc, from the first drained, shaky days of detox to the longer recovery period when sleep, mood, nutrition, and co-occurring mental health symptoms may still need treatment.
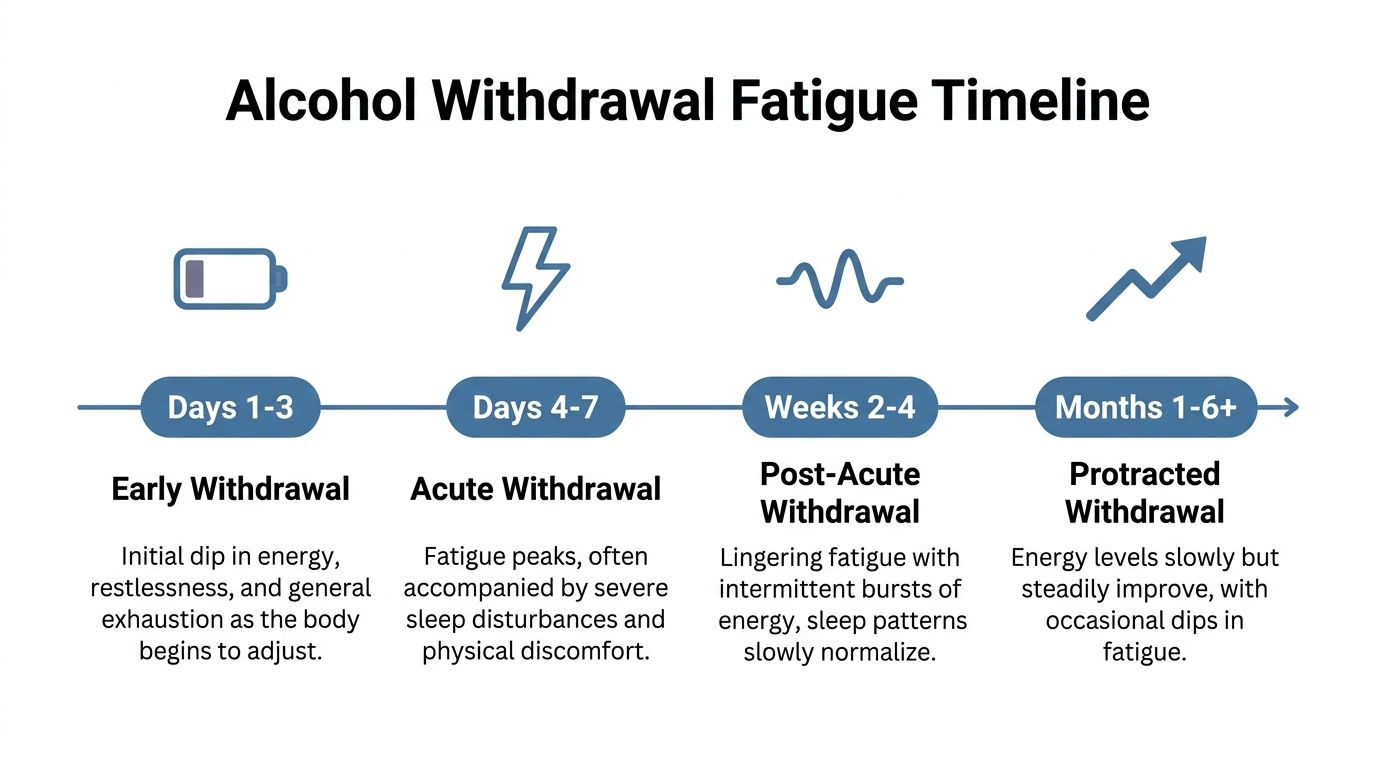
The Timeline of Alcohol Withdrawal Fatigue From Days to Months
You stop drinking, make it through the first night, and expect sleep to start fixing the problem. Then morning comes, and your body feels as if the battery never charged. By afternoon, you may feel shaky, drained, and unable to think clearly. A day later, the pattern may shift again.
That uneven pattern is common. Alcohol withdrawal fatigue usually comes in phases, not in a straight climb from bad to good. Knowing the general timeline can lower fear and help you tell the difference between expected healing, a warning sign, and a longer recovery issue that needs treatment.
If you want a broader overview of what the full withdrawal course can look like, this guide to alcohol detox timeline can help place fatigue in context.
Days 1 through 3
The first 24 to 72 hours are often the hardest. Many people feel very tired and physically unsteady at the same time. That combination can seem contradictory, but it fits the biology of withdrawal. The brain is trying to slow down after being pushed into an overactive state, while the body is also dealing with poor sleep, dehydration, stress hormones, and the physical strain of detox.
During this phase, fatigue often feels heavy and raw. Legs may feel weak. Simple decisions can take longer. A person may doze in short stretches without getting real rest.
Families sometimes misread this stage. Someone who is exhausted may still be at risk for worsening symptoms, especially if tremors, vomiting, confusion, or rising agitation are present.
| Phase | What tiredness often feels like | What can confuse people |
|---|---|---|
| Early acute withdrawal | Heavy, shaky, weak, mentally slowed | The person looks exhausted but still cannot get restorative sleep |
| Peak symptom window | Drained and overstimulated at the same time | Fatigue can appear even while medical risk is still rising |
Days 4 through 10
For many people, this is the mixed-signal stage.
The sharpest physical symptoms may begin to ease, but energy does not always come back with them. A person might wake up thinking, “I’m turning a corner,” then hit a wall by late afternoon. Sleep can remain broken. Mood can swing. Concentration may improve for a few hours and then drop again.
This is often where discouragement sets in. The outside crisis looks smaller, but the inside experience still feels unstable. That mismatch can trigger shame or impatience.
A helpful comparison is a city power grid after a major storm. The lights flicker back on in one block, then another, while some areas still go dark without warning. Early recovery can feel like that. Function is returning, but not evenly.
Weeks 2 through 6
By this point, many people expect to feel normal again. If they do not, they may wonder whether the fatigue means permanent damage, laziness, depression, or a medical problem no one has noticed.
Sometimes another health issue does need attention. Often, though, this stretch reflects post-acute withdrawal symptoms. The emergency phase has passed, but the brain and body are still recalibrating systems that affect sleep, stress response, mood, motivation, and mental clarity.
Common patterns in this window include:
- Hard mornings, even after spending enough time in bed
- Energy crashes during work, parenting, or errands
- Brain fog that comes and goes
- Irritability or anxiety that makes tiredness feel worse
- Short periods of feeling better, followed by a sudden dip
This stage is where generic detox advice often falls short. A person may no longer need the intensity of acute withdrawal management, but they may still need real treatment. In Dallas, dual-diagnosis care can make a major difference here because lingering fatigue is often tied to more than one problem at once. Sleep disruption, anxiety, depression, trauma symptoms, poor nutrition, and alcohol cravings can all feed each other.
Months 1 through 6 and beyond
For some people, fatigue fades steadily over the first month. For others, it lingers in waves for several months. That longer pattern is often grouped under PAWS, or post-acute withdrawal syndrome.
PAWS-related tiredness tends to look different from the first detox crash. The person may not feel acutely ill, but stamina is still low. Stress drains them faster. Concentration is less reliable. Sleep may improve and then suddenly worsen after a conflict, a poor week of eating, or a return of anxiety symptoms.
That does not mean recovery has stopped. It usually means recovery has moved into a deeper repair phase.
This is also the point where integrated treatment matters most. In Dallas, the strongest care plans do more than wait for energy to return on its own. They assess for depression, anxiety, trauma, and other co-occurring conditions, while also rebuilding the basics that support the nervous system: regular meals, hydration, sleep structure, medication support when appropriate, therapy, and relapse prevention. If a person has both alcohol use disorder and a mental health condition, treating only one often leaves fatigue in place.
A simple way to view the full timeline is this:
- Days 1 to 3: exhaustion mixed with physical withdrawal distress
- Days 4 to 10: partial improvement with unpredictable crashes
- Weeks 2 to 6: lingering fog, low energy, and mood-related fatigue
- Months 1 to 6 and beyond: waves of PAWS that often improve with structured dual-diagnosis treatment
The main message is reassuring. Fatigue after alcohol withdrawal can last longer than people expect, but it usually makes more sense once you see the timeline clearly. If you are in Dallas and your exhaustion feels intense, prolonged, or tangled up with anxiety, depression, insomnia, or cravings, that is not a sign to push harder alone. It is a sign to get the right level of help for the stage you are in.
Key Factors That Influence Withdrawal Severity
Two people can stop drinking on the same day and have very different withdrawal experiences. One may feel wrung out for a few days and gradually improve. Another may battle fatigue, panic, insomnia, and mental fog for much longer.
That difference usually comes from a mix of history, health, and mental health.
Alcohol history changes the picture
How long a person has been drinking and how heavily they’ve been drinking can affect how intense withdrawal tiredness feels. A longer pattern of alcohol use usually means the brain and body have spent more time adapting to alcohol’s presence.
That often leads to a rougher readjustment. The body has more repair work to do, and the nervous system may take longer to settle.
Mental health can prolong exhaustion
Co-occurring mental health conditions can make withdrawal fatigue much harder to shake. Anxiety can keep the nervous system activated. Depression can flatten motivation and energy. Trauma-related symptoms can disrupt sleep and increase physical tension.
Verified data shows that up to 75% of people with an alcohol use disorder and a comorbid mood disorder experience PAWS symptoms, including fatigue, that last 2 to 12 months longer than in those without, and only 12% of U.S. facilities offer the integrated dual diagnosis care needed to address this (New Found Life on alcohol withdrawal fatigue and healing).
This helps explain why some people say, “I stopped drinking, but I still feel terrible.” Alcohol may have been only part of the picture. If anxiety, depression, bipolar disorder, or PTSD are also present, fatigue can linger unless treatment addresses both conditions together.
When exhaustion keeps returning, the question isn’t only “How much did this person drink?” It’s also “What else is happening in the brain and body?”
Nutrition sleep and overall health matter
Withdrawal is tougher when the body starts from a depleted place.
A person who has been skipping meals, sleeping poorly, or living with other medical issues may have fewer reserves. Low appetite during detox can deepen weakness. Disturbed sleep can intensify brain fog. Dehydration can leave someone feeling faint, heavy, or headachy.
The following factors often shape severity:
- Nutritional depletion can worsen low energy and slow physical recovery.
- Sleep disruption can make tiredness feel constant even when someone spends more time in bed.
- Coexisting health problems can complicate what would otherwise be a more predictable detox process.
- Stress load at home can drain energy further, especially for parents, caregivers, or people trying to keep working through withdrawal.
For many families in Dallas and surrounding communities, the value of integrated treatment becomes clear. A person doesn’t need only a place to stop drinking. They may need medical support, sleep stabilization, therapy, nutrition support, and help treating anxiety or depression at the same time.
Safe At-Home Strategies to Manage Mild Fatigue
Mild fatigue can sometimes be supported at home, but only when symptoms are clearly mild and there’s no sign of dangerous alcohol withdrawal. Extreme shakiness, confusion, hallucinations, seizures, uncontrolled vomiting, or major distress require immediate medical care. Moderate to severe withdrawal should not be managed alone.
For someone with mild tiredness and no red flags, a few basic measures can help the body recover more steadily.
Supportive steps that may help
Hydration first. Small, regular sips of water or electrolyte-containing fluids can help when the body feels run down. Dehydration often makes weakness and headaches feel worse.
Simple balanced meals. Regular eating can matter even when appetite is low. A combination of protein and complex carbohydrates may feel easier on the body than long gaps without food.
Gentle movement instead of hard exercise. A short walk, light stretching, or a slow lap around the block is usually more realistic than pushing into strenuous workouts. Early recovery is not the time to “sweat it out.”
Low-pressure rest. Short rest periods can help, but all-day bedrest sometimes backfires by disrupting nighttime sleep even more.
Sleep routine support. A dark room, a steady bedtime, less screen exposure late at night, and a quiet sleep space can help the brain re-learn healthy sleep patterns. For readers looking for practical bedroom-focused ideas that may improve sleep quality for restful nights, that resource offers useful environmental tips.
A realistic example helps. Someone in East Dallas who feels washed out after stopping alcohol may do better with toast and eggs, water throughout the morning, a short walk in the afternoon, and an early quiet evening than with coffee, skipped meals, and a forced gym session.
When home management is not safe
Home care stops being appropriate when fatigue comes with signs that suggest dangerous withdrawal or severe instability.
A person should seek urgent medical help if they develop:
- Confusion or disorientation
- Hallucinations or severe agitation
- Seizure activity
- Inability to keep fluids down
- Rapid worsening after a brief period of improvement
Family members should trust what they’re seeing. If someone looks medically unwell, can’t stay oriented, or seems far more distressed than simple tiredness would explain, professional detox is the safer path. In alcohol withdrawal and tiredness can hide serious risk under a symptom that sounds deceptively ordinary.
Why Medical Detox in Dallas is the Safest Path to Recovery
A common Dallas scenario goes like this. Someone stops drinking, expects to feel shaky or anxious, then gets hit by something they did not expect. Heavy exhaustion. They sleep poorly, drag through the day, and assume they just need more willpower.
That assumption can be dangerous.
Fatigue during alcohol withdrawal is not just “being worn out.” It often reflects a brain and body trying to rebalance after alcohol has been acting like a brake on the nervous system for a long time. Once that brake is removed, the system can swing in the opposite direction. The result may include poor sleep, sweating, racing heart, anxiety, weakness, and mental fog all at once. In some people, the picture can worsen quickly.
Medical detox changes the setting from guesswork to observation. Instead of waiting to see whether exhaustion stays mild or turns into something more serious, a clinical team can track symptoms in real time, check vital signs, assess hydration, and respond early if the withdrawal pattern starts to escalate. As noted earlier, serious complications can emerge after the first day, which is one reason fatigue should be assessed in context rather than dismissed as a minor complaint.
Monitoring helps clinicians separate ordinary fatigue from dangerous change
Withdrawal rarely follows a perfectly straight line. A person may look only tired in the morning and become confused, agitated, or medically unstable later.
That is why supervised detox is safer. Clinicians are not only watching for dramatic events such as seizures. They are also watching for smaller warning signs that often show up first, such as rising blood pressure, worsening tremor, increasing agitation, inability to sleep, poor fluid intake, or a sudden change in orientation. Those details matter because severe withdrawal often develops as a progression, not as a single abrupt moment.
For families, this can be hard to judge at home. Exhaustion makes people look quiet and still. Severe withdrawal can begin that way too.
Treatment supports the whole system, not just one symptom
A tired body in withdrawal usually needs more than rest. It may need fluids, food, sleep support, symptom-guided medication, and repeated reassessment as the next several hours unfold.
Medical detox can provide:
- Medication support to reduce withdrawal intensity and calm an overactive nervous system
- Hydration and nutrition to address the depletion that often worsens weakness, shakiness, and brain fog
- Sleep support so exhaustion is not made worse by another night of fragmented rest
- Ongoing clinical reassessment because withdrawal symptoms can shift from hour to hour
Medication decisions are individualized. Some people need close symptom management for only a short period. Others need a more structured taper and monitoring plan, especially if they have a history of severe withdrawal, heavy daily alcohol use, or co-occurring medical problems. Readers who want a clearer explanation of treatment options can review this guide on the best medication for alcohol withdrawal.
The full fatigue timeline matters, especially when mental health is part of the picture
One of the biggest gaps in generic articles is that they stop at detox. In real clinical care, fatigue often has two phases. The first is acute withdrawal, when the body is in immediate chemical rebound. The second can come later, when sleep, mood, motivation, and energy remain unsettled for weeks or months. That longer stretch is often described as post-acute withdrawal syndrome, or PAWS.
PAWS can be confusing. People start to wonder whether they are failing at recovery, when in fact the brain may still be healing. If depression, anxiety, trauma, or bipolar symptoms are also present, the fatigue can feel even heavier and last longer. In that situation, treating detox as a stand-alone event misses the underlying problem.
Integrated dual-diagnosis care addresses both sides at once. Tru Dallas Detox & Recovery Center in Euless serves the wider Dallas area with medically supervised detox, 24/7 clinical monitoring, medication-assisted treatment, therapy, and support for co-occurring mental health conditions. That matters in practical terms. If panic is keeping someone awake, treatment can address panic and withdrawal together. If depression is flattening energy after the acute phase ends, follow-up care can be built into the plan instead of postponed until relapse risk grows.
A safer start often leads to a steadier recovery. When people understand why they feel so tired, and get care for both withdrawal and mental health at the same time, they are more likely to stay engaged through the acute phase and the longer healing period that can follow.
Take the First Step Toward Renewed Energy in Dallas
Alcohol withdrawal and tiredness can make recovery feel farther away than it really is. A person may feel weak, foggy, irritable, and discouraged, then assume they’ll never feel normal again. That conclusion is common, but it’s often wrong.
Withdrawal fatigue usually reflects a body and brain working hard to heal. Some people move through it in days. Others need support over a longer stretch, especially when sleep problems or mental health symptoms remain active. What matters most is not guessing alone.
For individuals and families in Dallas, Fort Worth, Euless, Plano, Irving, and nearby communities, the safer move is to treat heavy exhaustion after quitting alcohol as something worth assessing. If symptoms are strong, unpredictable, or frightening, medical detox can protect both safety and recovery.
Help is available now. A confidential call can answer questions, review symptoms, and help determine whether detox, inpatient treatment, or another level of care makes the most sense. Insurance verification can also help families move faster when timing matters.
Frequently Asked Questions About Alcohol Withdrawal
Some concerns tend to come up late at night, after a hard day, or right before someone is ready to ask for help. Quick answers can make the next step feel more possible.
The verified data notes that in post-acute withdrawal syndrome, fatigue can continue alongside sleep problems and cognitive dysfunction, often becoming more noticeable in weeks 2 through 8 because of neural rewiring and sleep debt repayment (Nova Recovery Center on alcohol fatigue syndrome).
Common Questions About Withdrawal and Recovery
| Question | Answer |
|---|---|
| Is it normal to feel exhausted after quitting alcohol? | Yes. Exhaustion is a common withdrawal experience. The key question is severity. Mild fatigue can happen in normal recovery, but severe symptoms need medical assessment. |
| How can family members help? | They can watch for warning signs, help reduce stimulation, encourage hydration and food, and seek urgent help if confusion, hallucinations, or seizures appear. |
| When does tiredness become a warning sign? | It becomes more concerning when it comes with disorientation, inability to sleep for long periods, severe agitation, hallucinations, seizure activity, or a sudden medical decline. |
| Can someone still need treatment after detox? | Yes. Many people need ongoing care because low energy, mood symptoms, cravings, and sleep disruption can continue after the acute phase. |
| Will insurance questions delay help? | They shouldn’t. Many treatment programs can verify insurance and explain options quickly so families can make a clear decision. |
Recovery often starts with one practical step. A phone call, a symptom review, or an insurance check can turn confusion into a plan.
If alcohol withdrawal and tiredness are making daily life feel unmanageable, support is available through Tru Dallas Detox & Recovery Center. A confidential conversation can help clarify symptoms, discuss detox and dual diagnosis options, verify insurance, and identify the safest next step for recovery in the Dallas-Fort Worth area.