A person in Dallas may start by telling themselves the drinking is still manageable. It is just a few drinks in Uptown after work. Just weekend relief. Just something to take the edge off before bed. Then the pattern shifts. The nights get later. The mornings get harder. Promises to cut back last a day or two, then stress, loneliness, guilt, or habit pulls everything back into the same loop.
That is often when many people begin looking for real help. Not vague advice. Not shame. A way to understand why alcohol keeps taking over, and what to do next.
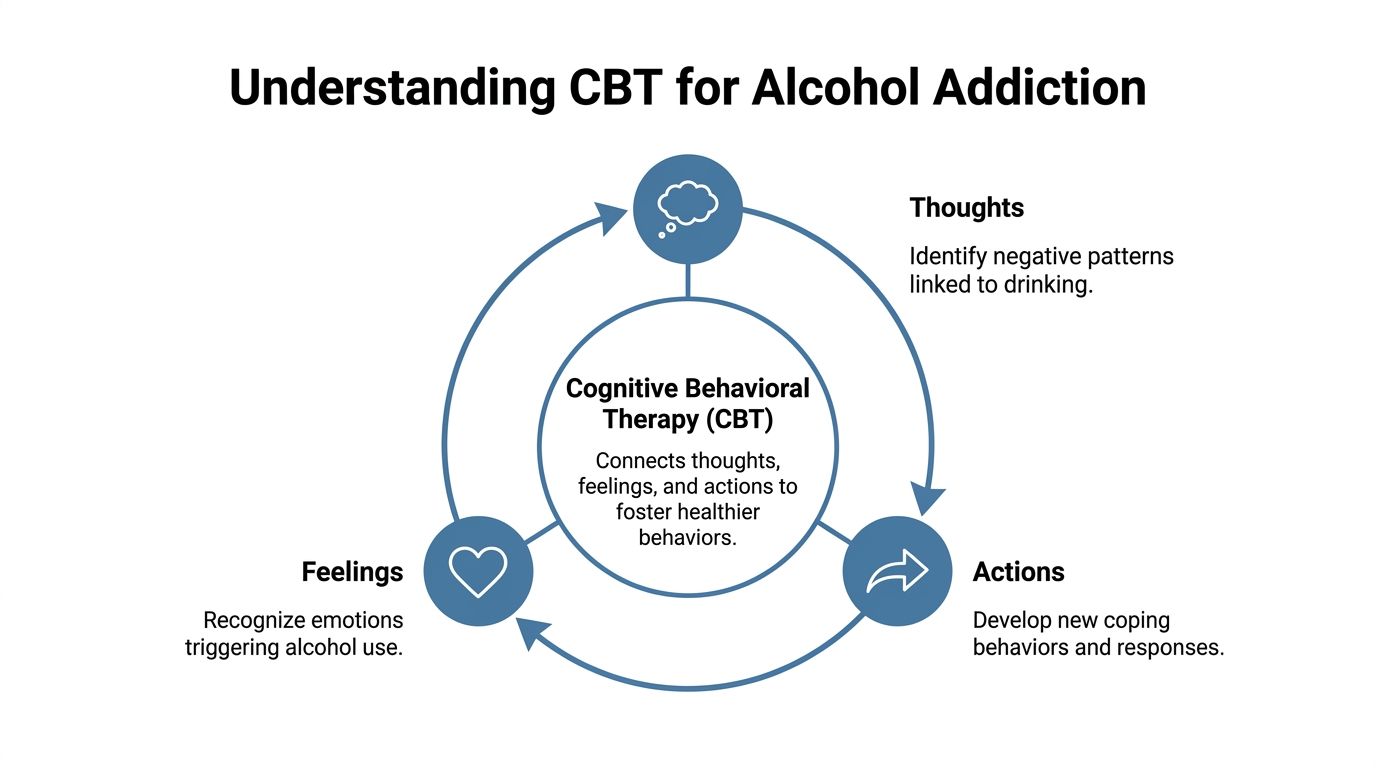
Cognitive behavioral therapy for alcohol addiction gives that process structure. It helps people identify the thoughts, emotions, triggers, and routines that keep drinking in place. Then it teaches practical ways to interrupt those patterns and build healthier ones. For people searching for addiction treatment in Dallas, CBT often becomes one of the clearest paths from crisis to daily stability.
Table of Contents
- The Cycle of Alcohol Use and the Search for a Way Out
- What Is CBT and Why It Works for Alcohol Addiction
- Core CBT Techniques to Reclaim Control from Alcohol
- The Proven Effectiveness of CBT in Addiction Treatment
- How CBT is Delivered at Leading Dallas Treatment Centers
- Your Recovery Journey with CBT at Tru Dallas
- Frequently Asked Questions About CBT for Alcoholism
The Cycle of Alcohol Use and the Search for a Way Out
In the Dallas-Fort Worth area, alcohol can subtly weave itself into daily life. A person may drink after a stressful commute on I-35, during dinners in Las Colinas, at social events in Downtown Dallas, or alone at home after everyone else goes to sleep. At first, it can look like stress relief. Over time, it starts to feel like survival.
The painful part is not only the drinking itself. It is the cycle around it. A person feels overwhelmed, drinks to cope, feels temporary relief, then wakes up with regret, conflict, physical discomfort, or fear. Those feelings become new triggers. The cycle starts again.
Family members often see the same pattern from the outside. They notice broken promises, mood changes, isolation, or a growing sense that alcohol is now calling the shots. The person drinking often feels ashamed because they still care about their work, relationships, and future. They may want help and still feel terrified to ask for it.
That fear makes sense. Many people assume treatment means being judged, losing control, or being told to “try harder.” Effective care does not work that way. Recovery begins when a person can see the pattern clearly and learn how to respond differently.
A helpful starting point is understanding the broader recovery process for alcohol addiction. That journey usually includes stabilization, therapy, skill-building, and aftercare. CBT fits into that path by helping people understand what keeps the cycle going.
Key takeaway: Alcohol problems often continue because the same triggers, thoughts, emotions, and routines keep repeating. CBT helps break that repetition.
For many people seeking a Dallas detox center or rehab program, this is the first real sign of hope. The problem is not that they are weak. The problem is that they are stuck in a learned pattern. Learned patterns can be changed.
What Is CBT and Why It Works for Alcohol Addiction
Cognitive behavioral therapy, often called CBT, is a structured form of therapy that helps people understand the connection between what they think, what they feel, and what they do. In alcohol treatment, that matters because drinking rarely happens in a vacuum. It usually follows a chain.
The automatic loop
A simple way to understand CBT is to picture an automatic loop:
| Part of the loop | Common example tied to alcohol |
|---|---|
| Thought | “This day was awful. A drink is the only way to calm down.” |
| Feeling | Anxiety, frustration, loneliness, anger |
| Action | Drinking, isolating, giving up on the evening |
| Aftereffect | Temporary relief, then guilt, conflict, cravings, or more stress |
Once this loop repeats enough times, it starts to feel automatic. A person may not even notice the thought that comes before the urge. They just feel pulled toward alcohol.
CBT slows that moment down. It teaches a person to catch the thought, name the feeling, and choose a different response before the behavior takes over.
CBT focuses on patterns, not blame
Readers often get confused at this point. CBT is not about telling someone that drinking is “all in their head.” It is not positive thinking. It is not pretending cravings are imaginary.
It is a practical method for spotting the mental habits that keep alcohol in the center of life. One person may drink after the thought, “I already messed up today, so it doesn’t matter.” Another may drink after, “I cannot handle this anxiety unless I numb it.” CBT helps examine whether those thoughts are accurate, helpful, or distorted.
That can feel especially important for people who have started to worry about reward, craving, and motivation in the brain. For a plain-language explanation of how those systems influence behavior, this guide on dopamine and motivation can help clarify why short-term relief becomes so compelling.
Why this approach helps people change
CBT works because it turns recovery into a set of learnable skills. A person does not have to wake up with perfect willpower. They can learn how to:
- Notice triggers: specific places, people, times of day, or emotional states.
- Question automatic thoughts: especially the ones that make alcohol seem necessary.
- Practice replacement behaviors: calling support, leaving a risky setting, eating, resting, journaling, or using a coping exercise.
- Prepare for high-risk moments: social pressure, conflict, boredom, celebrations, and loneliness.
The evidence behind CBT for alcohol use disorder is strong. A landmark review found that CBT produced 15% to 26% better outcomes than minimal or no treatment for reducing alcohol use, and the large Project MATCH trial found that people in CBT increased abstinent days by about 25% to 30% on average (Journal of Consulting and Clinical Psychology meta-analysis and Project MATCH findings).
Those numbers matter, but the day-to-day meaning matters more. CBT gives people a way to respond differently on Tuesday afternoon, Friday night, and the next difficult holiday. This makes recovery real.
Core CBT Techniques to Reclaim Control from Alcohol
The most useful way to think about CBT is as a recovery toolkit. Each skill targets a different part of the drinking cycle. Some help before a craving starts. Some help in the middle of an urge. Some help after a difficult moment, so one lapse does not become a full return to old patterns.
Functional analysis
This is one of the most important CBT tools for alcohol addiction. Functional analysis means looking closely at what happened before, during, and after drinking.
A therapist may ask questions like these:
- Before drinking: What happened that day? Who was around? What emotion showed up first?
- During drinking: What did alcohol seem to promise in that moment?
- After drinking: What were the consequences physically, emotionally, and relationally?
A Dallas example might look like this. A person leaves work exhausted, argues with a partner by text during the drive home, stops at a store out of habit, and tells themselves they deserve relief. The alcohol lowers tension for a short time. Later, sleep gets worse, the argument escalates, and the next day begins with guilt and a stronger urge to escape again.
When that chain is written out, the drinking stops looking random. It becomes something that follows specific cues.
Tip: The goal is not to prove that someone is failing. The goal is to identify the exact points where a different choice can be inserted.
Cognitive restructuring
After identifying the pattern, CBT helps challenge the thought that keeps the behavior alive. This is called cognitive restructuring.
Common alcohol-related thoughts include:
- “I need a drink to relax.”
- “If cravings start, they will just get worse until I give in.”
- “I already slipped, so the whole week is ruined.”
- “Other people can handle life. Something is wrong with me.”
A therapist helps the person test those thoughts. Is alcohol the only way they have ever relaxed, or just the most familiar one? Does a craving always keep rising, or does it peak and pass? Does one mistake erase progress, or is that all-or-nothing thinking?
Thoughts shape behavior. If a person believes they are powerless, they act powerless. If they learn to replace that thought with something more accurate, such as “This urge is uncomfortable, but it will pass if it is not fed,” the next action can change.
For people who feel panicked by urges or emotional overwhelm, this can also connect to a deeper fear that everything is spiraling. Some readers find it helpful to explore the emotional side of that experience through this article on Stop the Fear of Losing Control.
Skills practice for cravings and social pressure
CBT is not only about insight. It includes rehearsal.
A person in recovery may know alcohol is harmful and still freeze when a craving hits or when friends push drinks at a birthday dinner in Deep Ellum. Skills practice prepares for those moments.
Three examples matter a lot:
Urge surfing
Instead of fighting a craving or obeying it, the person notices it like a wave. The urge rises, peaks, and passes. Attention goes to breathing, body sensations, and staying in the present moment without acting.Drink refusal practice
Short responses are rehearsed ahead of time.
“No thanks.”
“Not tonight.”
“I’m good with this.”
Rehearsal reduces panic when the moment is real.Behavioral substitution
The person builds an action list for high-risk times. That might include leaving an event early, calling a support person, eating a full meal before socializing, changing the drive home, or keeping the evening planned hour by hour.
Readers who want a closer look at how this therapy is used in substance use treatment can learn more about CBT for addiction.
When CBT is combined with medication support
CBT teaches coping skills. Medication can help reduce the pull of cravings for some people. Research reviews have found that combining CBT with Medication-Assisted Treatment can produce larger and more durable effects than either approach alone (evidence review on CBT and pharmacotherapy for alcohol and drug use disorders).
That does not mean everyone needs medication. It means treatment can be matched to the person. Someone with intense cravings, repeated relapse, or a co-occurring mental health condition may benefit from both.
This is also why a quality Dallas alcohol rehab program should not treat therapy and medical support as separate worlds. The strongest care plan often combines them.
The Proven Effectiveness of CBT in Addiction Treatment
Many therapies promise change. CBT has earned trust in addiction treatment because it has been studied carefully and used across many levels of care.
Why clinicians rely on CBT
CBT is widely used because it addresses the daily mechanics of addiction. It helps people identify triggers, examine distorted thinking, tolerate distress, and build routines that support sobriety. Those are not abstract goals. They affect what someone does after a hard phone call, at the end of a lonely evening, or during a conflict at home.
Its value becomes even clearer when alcohol use is tied to depression or anxiety. In one study involving people with depression and alcohol-related problems, 37% of those who received a CBT component had no heavy drinking days, compared with 9% in treatment as usual (review discussing CBT and co-occurring mood disorders).
That finding matters because many people in need of addiction treatment in Dallas are not only fighting alcohol. They are also carrying hopelessness, panic, numbness, grief, or extreme mood swings.
CBT and dual diagnosis care
Dual diagnosis treatment becomes essential here. If alcohol is being used to blunt anxiety, escape depression, or cope with unstable mood, then treating only the drinking leaves part of the problem untouched.
CBT helps on both sides of that picture. It can teach a person to challenge thoughts like:
- “Nothing is going to get better anyway.”
- “If anxiety shows up, alcohol is the only thing that works.”
- “One bad day means total failure.”
It also gives structure to behavior. Sleep routines, coping plans, communication skills, trigger logs, and relapse prevention work can support both mood stability and sobriety.
Key takeaway: CBT is not only about stopping alcohol. It helps people build a more stable way of responding to stress, emotion, and self-criticism.
There are still areas where the data is more limited, especially for specific conditions such as bipolar disorder. That does not make CBT unhelpful. It means treatment should be personalized, careful, and integrated with mental health care rather than forced into a one-size-fits-all model.
For many families, this is the moment when treatment starts to make sense. The drinking is not separate from the emotional pain. Good therapy addresses both.
How CBT is Delivered at Leading Dallas Treatment Centers
People often picture therapy as one person sitting on a couch, talking about childhood for an hour. CBT for alcohol addiction can look very different. It is usually more active, more practical, and more customized to the person’s stage of recovery.
Individual CBT
In individual sessions, a therapist and client work closely on personal triggers, thought patterns, and relapse risks. This format can be especially useful when the drinking is tied to trauma, shame, severe anxiety, depression, family conflict, or a highly specific routine.
The benefit of one-on-one work is depth. A person can say the quiet part out loud without worrying about a room full of strangers. That includes thoughts such as, “I drink most when I feel rejected,” or “I start planning a relapse before I even realize I am upset.”
Individual CBT often focuses on:
- Personal triggers: work pressure, grief, conflict, isolation, boredom
- Private thought patterns: self-criticism, hopelessness, all-or-nothing thinking
- Targeted coping plans: customized steps for evenings, weekends, travel, or family events
Group CBT
Group settings give people a different kind of support. They hear how others describe cravings, rationalizations, and setbacks. That shared recognition can reduce shame quickly.
A strong group does more than offer encouragement. It teaches skills, invites practice, and helps participants test new responses out loud. Emerging research also suggests that combining CBT with therapies such as Motivational Interviewing in group care can improve outcomes for some people in outpatient treatment (discussion of CBT delivery options and group applications).
Common strengths of group work include:
- Shared accountability: other people notice patterns and progress.
- Practice in real time: refusal skills and coping statements can be rehearsed with feedback.
- Reduced isolation: a person learns they are not the only one who has hidden bottles, broken promises, or feared weekends.
Choosing the right format
There is no single perfect format for every person in Dallas or Fort Worth. The best match depends on symptoms, living situation, mental health needs, medical history, motivation, and recovery environment.
A simple comparison can help:
| Format | Often helpful when | Main strength |
|---|---|---|
| Individual CBT | The person needs privacy or has complex mental health concerns | Highly customized work |
| Group CBT | The person benefits from peer support and shared practice | Connection and accountability |
| Combined approach | The person needs both depth and community | Balanced support |
Many programs also place CBT inside a broader level of care, such as detox, residential rehab, partial hospitalization, or intensive outpatient treatment. People comparing options may find it helpful to understand how IOP programs in Dallas, TX fit into longer-term recovery.
In practice, treatment works best when the format fits the person, not the other way around.
Your Recovery Journey with CBT at Tru Dallas
It is 2 a.m. in Dallas, and someone has made the decision they have been putting off for months. They are scared to stop drinking, unsure what treatment will feel like, and worried they have already waited too long. The next steps matter most when life feels that unsteady.
Recovery usually unfolds in a clear sequence. First, the body has to settle. Then the mind can start learning new ways to respond to stress, cravings, and old habits. CBT supports that process from early treatment through daily life after discharge.
Step one starts with safety
For many people, alcohol withdrawal is not just uncomfortable. It can be dangerous. That is why the journey often begins with supervised detox instead of trying to quit alone at home.
During detox, medical staff watch for withdrawal symptoms, help manage discomfort, and work to stabilize sleep, hydration, blood pressure, and overall safety. CBT works best when the brain and body are no longer in acute withdrawal. A person in the middle of shaking, panic, nausea, or confusion is trying to survive the moment, not absorb therapy skills.
A simple way to understand this is to picture a smoke alarm that keeps going off. Detox helps quiet the emergency signal. Once that alarm settles down, CBT can teach the person what keeps setting it off and how to respond differently next time.
No one needs to arrive with a perfect plan. They only need a safe starting point.
Step two builds real-world coping skills
Once a person is medically stable, therapy becomes more practical and more effective. This is the stage where CBT starts turning fear into a plan.
At Tru Dallas Detox & Recovery Center, care may include medically supervised detox, inpatient or outpatient rehab, Medication-Assisted Treatment, dual diagnosis services, individual therapy, group counseling, and aftercare planning. Within that structure, CBT helps connect the dots between thoughts, emotions, situations, and drinking behavior.
Instead of talking about alcohol use in vague terms, CBT gets specific. A therapist may help someone notice that the urge to drink rises after an argument, during the drive home on I-35, or when the house feels too quiet at night. Those details matter because recovery gets stronger when the person knows exactly what they are dealing with.
Common CBT work in this phase includes:
- Trigger mapping: identifying the people, places, moods, and routines linked to drinking
- Craving planning: choosing what to do in the first few minutes of an urge, before autopilot takes over
- Relapse prevention: preparing for high-risk situations such as weekends, holidays, work stress, conflict, boredom, or isolation
- Mental health support: treating anxiety, depression, trauma, or mood symptoms that may be fueling alcohol use
CBT works like physical therapy for the mind. Repeating new responses may feel awkward at first, but practice builds strength. Over time, the pause between urge and action gets wider, and that small gap can protect sobriety.
Helpful reminder: Recovery does not require feeling strong every day. It requires knowing what to do on the hard days.
Step three turns treatment gains into daily recovery
Leaving treatment can feel encouraging and unsettling at the same time. The structure is lighter. Old routines are nearby. Everyday life in the DFW area returns quickly, including work pressure, family stress, traffic, loneliness, and easy access to alcohol.
That is why aftercare matters. The goal is not only to complete treatment. The goal is to keep using CBT skills in ordinary moments, when no one is standing beside the person telling them what to do.
An aftercare plan may include ongoing therapy, support groups, outpatient care, medication follow-up, sober living referrals, family work, and digital tools that reinforce coping skills between sessions. Research from Yale found that a web-based CBT program increased percentage of days abstinent across eight months (Yale report on digital CBT for alcohol use disorder). That kind of support can help a person keep practicing the same skills they started learning in treatment.
A useful plan answers practical questions before a crisis starts:
- Who can the person call when cravings spike?
- What is the plan if anxiety, depression, or insomnia returns?
- How will evenings and weekends stay structured?
- What support continues after discharge?
For someone looking for help in Dallas, the process should not feel mysterious. It should feel doable. One safe step, then the next, then the next.
Frequently Asked Questions About CBT for Alcoholism
How long does CBT for alcohol addiction take
There is no single timeline that fits everyone. Some people begin CBT during detox or residential treatment and continue it in outpatient care. Others start in an outpatient setting if they are already medically stable.
The right length depends on several factors, including severity of alcohol use, relapse history, mental health symptoms, home support, and whether the person needs detox, Medication-Assisted Treatment, or dual diagnosis care. What matters most is consistent practice. CBT works best when the skills are used between sessions, not only discussed during them.
Will PPO insurance cover treatment
Coverage depends on the specific plan, level of care, and medical necessity. Many people in the Dallas area feel overwhelmed by insurance questions, especially when they are already dealing with a crisis.
The simplest next step is to verify benefits directly with the treatment provider. That can help clarify whether detox, inpatient rehab, outpatient care, therapy, or medication support may be covered. Families should not assume they have to solve all of that alone before making a call.
What if there is a relapse or setback
A setback does not erase progress. In CBT, a relapse or slip is treated as important information, not proof that treatment failed.
The focus shifts to questions such as:
- What happened right before the drinking started?
- What thought or emotion went unaddressed?
- What part of the plan needs to be strengthened?
- What support was missing in that moment?
That approach reduces shame and increases learning. A person can examine the event, repair what needs repair, and return to treatment with more insight than before.
Important perspective: Recovery is often strengthened by honest review after a setback. Shame keeps people stuck. Analysis helps people move forward.
Is CBT enough on its own
Sometimes CBT is a central part of treatment, but it is not always the only service a person needs. Someone with significant withdrawal symptoms may need detox first. Someone with strong cravings may benefit from medication support. Someone with depression, anxiety, or bipolar symptoms may need integrated mental health care as well.
A good treatment plan is built around the whole person. CBT may work alongside:
- Medical detox
- Psychiatric care
- Medication-Assisted Treatment
- Group counseling
- Family support
- Outpatient or aftercare services
That is especially true when alcohol addiction has affected work, parenting, physical health, or safety. The goal is not to choose one “perfect” therapy. The goal is to create enough support for recovery to hold.
What if a person feels ashamed to ask for help
That fear is common. Many people wait because they believe they should be able to fix the problem privately, or because they worry about being judged.
Treatment should reduce shame, not increase it. CBT is often helpful here because it puts language around the pattern. Instead of “What is wrong with this person?” the better question becomes “What keeps happening, and how can that cycle be interrupted?” That shift alone can make asking for help feel possible.
Can family members be involved
Often, yes. Family involvement depends on the program and the client’s wishes, but loved ones can play an important role in understanding triggers, supporting healthy routines, and responding more effectively to setbacks.
Families also need guidance. They may be exhausted, frightened, or unsure where support ends and enabling begins. Good treatment helps the whole system become healthier, not only the person who has been drinking.
For anyone in Dallas or the surrounding DFW area who is frightened by alcohol use and unsure what to do next, reaching out for help can be the first turning point. Tru Dallas Detox & Recovery Center offers confidential support, insurance verification for many PPO plans, and a path from medically supervised detox to ongoing treatment and aftercare. A call can answer questions, clarify options, and help determine the safest next step.